Scabies in Kids: What It Looks Like and How to Treat It
Sarah Mitchell
Sarah Mitchell is a Registered Pediatric Nurse and a mother of three who has spent over a decade helping families navigate the beautiful, chaotic early years of childhood. She combines evidence-based medical knowledge with real-world parenting experience to offer practical, compassionate advice. At Awesome Parent, Sarah's mission is to help exhausted parents find solutions, trust their instincts, and finally get some sleep.
If your child has a suddenly super itchy rash that seems worse at night, and you are wondering, “Is this scabies?” you are not alone.
I saw it regularly as a pediatric triage nurse, and it can absolutely make families miserable until it’s properly treated.
The good news: scabies is very treatable. The tricky part is recognizing it (it can look like eczema, bug bites, or allergies), and treating everyone who needs treatment at the same time so it doesn’t boomerang right back through your household.
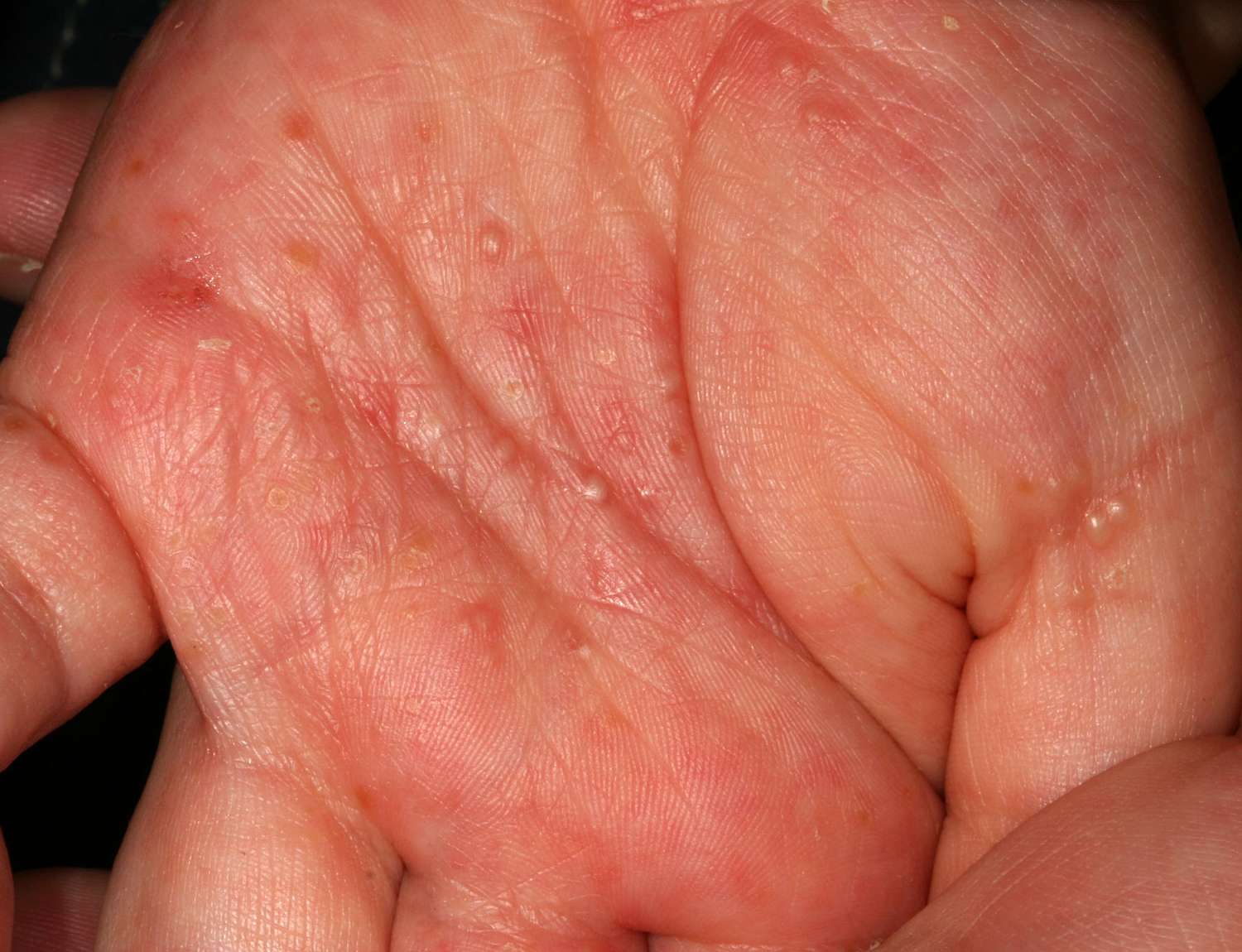
What is scabies?
Scabies is a skin infestation caused by a tiny mite called Sarcoptes scabiei. The mite burrows into the top layer of skin and triggers an allergic-type reaction. That reaction is what causes the intense itching and rash.
Important parent note: scabies has nothing to do with being dirty. Kids get scabies because kids are experts at close contact. They cuddle, wrestle, pile on the same couch, and share blankets like it is their job.
What it looks like
The itch (often the biggest clue)
Scabies itch is typically:
- Very itchy, sometimes dramatically so
- Worse at night (many parents notice it most at bedtime)
- Out of proportion to how “mild” the rash might look
The rash
In children, scabies often appears as:
- Small red bumps or tiny pimples
- Clusters of bumps that look like bug bites
- Scratch marks and scabs from itching
- Sometimes tiny blisters, especially in younger kids
Burrows (the classic sign)
Burrows are short, thin, slightly raised lines in the skin. They can look like faint pencil marks or tiny tracks. They are not always easy to see, especially if your child has been scratching.
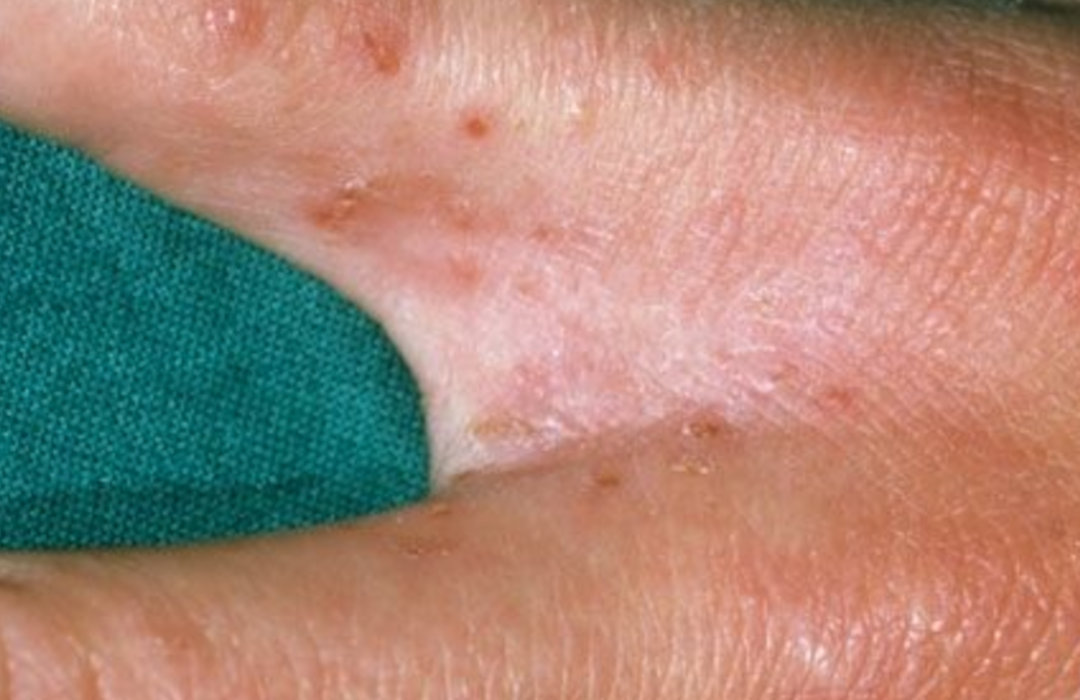
Common locations
Scabies has favorite hangouts. In kids, it commonly shows up on:
- Between the fingers and on the sides of fingers
- Wrists
- Elbows
- Armpits
- Waistline and belly button area
- Groin and inner thighs
- Buttocks
- Ankles and feet
In babies and toddlers, scabies can also affect the scalp, face, neck, palms, and soles, which is less common in older kids and adults.
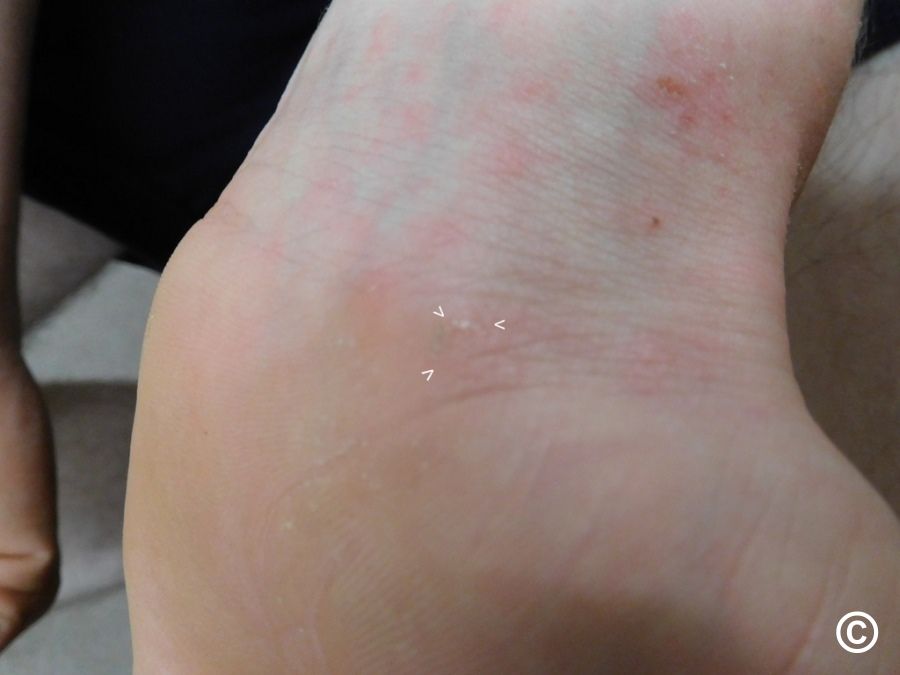
How it spreads
Scabies spreads mostly through prolonged skin-to-skin contact. Think: bed-sharing, snuggling during a movie, wrestling, helping with bathing, or close play at daycare. It is usually not from a quick hug or a brief handshake.
Less commonly, it can spread through shared items like:
- Bedding and blankets
- Towels
- Recently worn clothing
Off the body, scabies mites typically do not survive long. In most household situations, they live up to about 2 to 3 days (around 72 hours) away from human skin. Temperature and humidity matter, and fomite spread is more of a concern in crusted scabies (more on that below).
When to call the pediatrician
Call your child’s clinician if:
- Your child has an itchy rash that is worsening or spreading
- Multiple family members are itchy
- The rash is in classic scabies locations (hands, wrists, waistline)
- Your child has signs of skin infection from scratching (increasing redness, warmth, swelling, pus, honey-colored crusts, fever)
- Your child is under 2 months old (treatment choices differ)
Diagnosis is often made by looking at the rash pattern and symptoms. Sometimes clinicians do a skin scraping, but many cases are diagnosed clinically.
One more helpful timeline detail: after a first exposure, symptoms can take about 2 to 6 weeks to show up. With reinfestation, symptoms can appear much faster.
Treatment
Scabies usually requires prescription treatment. Over-the-counter anti-itch creams may soothe symptoms, but they do not kill the mites.
Permethrin 5% cream
Permethrin 5% cream is a very common first-choice medication for scabies in children (and adults). It kills the mites and is generally well tolerated.
Typical instructions (follow your prescriber’s directions exactly):
- Apply to clean, dry skin.
- Cover the body from the neck down.
- In older children and adults, the face and scalp are usually avoided unless your clinician specifically tells you otherwise.
- In infants and some toddlers, the clinician may instruct you to include the scalp/hairline, temples, and forehead (avoiding eyes and mouth).
- Pay special attention to: between fingers and toes, under nails, wrists, armpits, belly button, buttocks, and groin.
- Do not forget hands and feet.
- Leave it on for the recommended time (often 8 to 14 hours), then wash it off.
- Reapply to hands if your child washes their hands during the treatment window (this is a very common real-world reason treatments fail).
- A second treatment is often recommended about 1 week later to kill newly hatched mites.
Pro tip from the clinic: scabies treatment fails more often from missed areas than from “strong enough medicine.” Take your time, and remember the hands, feet, and under nails. Trim nails short and gently clean under them if you can, since mites and eggs can hide there.
Treat close contacts
This is the make-or-break step. Household members and close contacts may need treatment even if they are not itchy yet, because symptoms can take weeks to show up after the first exposure.
Ask your child’s clinician who should be treated, but in many cases this includes:
- Everyone living in the home
- Regular caregivers who have close physical contact
- Sleepover or bed-sharing contacts
Other prescription options
If permethrin is not appropriate or not working, clinicians may consider other medications such as oral ivermectin (often for older children and adults, depending on age and weight) or other topical agents. Many guidelines avoid ivermectin in children under about 15 kg, and it is generally not used in pregnancy unless a clinician determines the benefits outweigh risks. These decisions are individualized, especially in young children, pregnant caregivers, or medically complex kids.
Why treatment fails
If symptoms are not improving, these are the most common culprits:
- Missed areas (finger webs, under nails, buttocks, groin, feet)
- Not treating all close contacts at the same time
- Handwashing during the treatment window without reapplying to hands
- Not doing the second treatment when it is recommended
- Re-exposure from an untreated contact (including outside the home)
- The rash was something else (eczema, insect bites, viral rash)
Still itching after treatment?
Here is the part that makes parents doubt themselves: itching can continue for 2 to 4 weeks after successful treatment, and sometimes longer. This is called post-scabetic itch, and it happens because the skin is still reacting as it heals, even after the mites are gone.
What can help (ask your clinician what’s appropriate for your child):
- Fragrance-free moisturizer
- Cool compresses
- Short nails to reduce skin damage from scratching
- An oral antihistamine at bedtime for itch relief, if recommended
- A mild topical steroid for inflammation, if prescribed
What should not happen: brand new burrows, rapidly spreading bumps after the expected timeframe, or multiple untreated contacts developing symptoms. If that is happening, call the pediatrician and discuss reinfestation or an alternate diagnosis.
Cleaning your home
You do not need to deep-clean your entire house like you are preparing for a hazmat team. Focus on items that had close contact with skin in the last few days.
On day 1
- Wash bedding, pajamas, towels, and clothes worn recently in hot water, then dry on high heat.
- Items that cannot be washed can be sealed in a plastic bag for at least 3 days (about 72 hours).
- If you want to be extra cautious, some families choose to bag items longer (up to a week), but in typical household scabies this is usually not necessary.
- Vacuum carpets and upholstered furniture if your child spends lots of time there. Routine vacuuming is enough.
A common question I get: do you need to throw away stuffed animals? Almost never. Bagging them for a few days is usually sufficient if they cannot be washed and dried on heat.

School and daycare
Policies vary a bit by location, but a common standard is:
- Kids can usually return to daycare or school after starting and completing the first treatment application, often the next day, as long as they are otherwise well and it aligns with school or daycare policy.
Because scabies is contagious through close contact, notify the school or daycare so they can follow their health policy and watch for additional cases. This is not about blame. It is about stopping the spread so you are not dealing with round two.
Scabies vs. other rashes
Scabies vs. eczema
Eczema can be itchy and patchy, and it often shows up in skin creases. Scabies tends to have tiny bumps in classic locations like finger webs and wrists, with itch that is often worse at night and may affect multiple family members.
Scabies vs. bedbug bites
Bedbug bites often show up on exposed skin and may appear in lines or clusters. Scabies commonly affects hands and wrists and can show burrows. Both can itch a lot. If you suspect bedbugs, check sleeping areas and talk to your clinician if the rash pattern is unclear.
Scabies vs. impetigo
Impetigo often causes honey-colored crusts and can spread quickly, especially around the nose and mouth. Scabies can lead to secondary infection from scratching, so sometimes kids have both and need treatment for both.
Crusted scabies (rare)
Crusted scabies is uncommon in healthy children, but it matters because it is much more contagious and can spread more through shared items. It can look like thick crusting or scaling, sometimes with less obvious itching. If your child is immunocompromised, medically fragile, or has a severe crusted rash, call the clinician promptly. Treatment and cleaning guidance can be different.
When to seek urgent care
Scabies itself is rarely an emergency, but seek same-day care if your child has:
- Fever with a rapidly worsening rash
- Spreading redness, warmth, swelling, or significant pain (possible skin infection)
- Signs of dehydration or lethargy
- Rash involving the eyes with swelling or drainage
A calm plan for tonight
If you are reading this during a late-night itch spiral, here is a practical next step list:
- Take clear photos of the rash in good light (hands, wrists, waistline, any burrow-like lines).
- Call your pediatrician for an evaluation and prescription guidance.
- If scabies is diagnosed, plan a household treatment night and do the laundry and bagging routine the same day.
- Expect itch to improve gradually, not instantly, and check in if symptoms are not trending better over the next couple weeks.
You are not failing because this showed up in your home. Scabies is a nuisance, not a moral judgment. With the right treatment and a little coordination, it is very fixable.
Medical disclaimer
This article provides general educational information and is not a substitute for medical advice, diagnosis, or treatment. Always follow your child’s clinician’s guidance for medication use and return-to-school recommendations.