Scabies vs Eczema in Kids: How to Tell the Difference
Sarah Mitchell
Sarah Mitchell is a Registered Pediatric Nurse and a mother of three who has spent over a decade helping families navigate the beautiful, chaotic early years of childhood. She combines evidence-based medical knowledge with real-world parenting experience to offer practical, compassionate advice. At Awesome Parent, Sarah's mission is to help exhausted parents find solutions, trust their instincts, and finally get some sleep.
If you are staring at your child’s itchy skin at 2 AM wondering, “Is this scabies or just eczema?” you are not alone. These two can look frustratingly similar at first glance, but a few clues usually point you in the right direction. The big difference is this: scabies is caused by mites and spreads easily through close contact, while eczema is an inflammatory skin condition and is not contagious.
I will walk you through what to look for, what you can safely do at home, what to avoid, and when it is time to get urgent help.
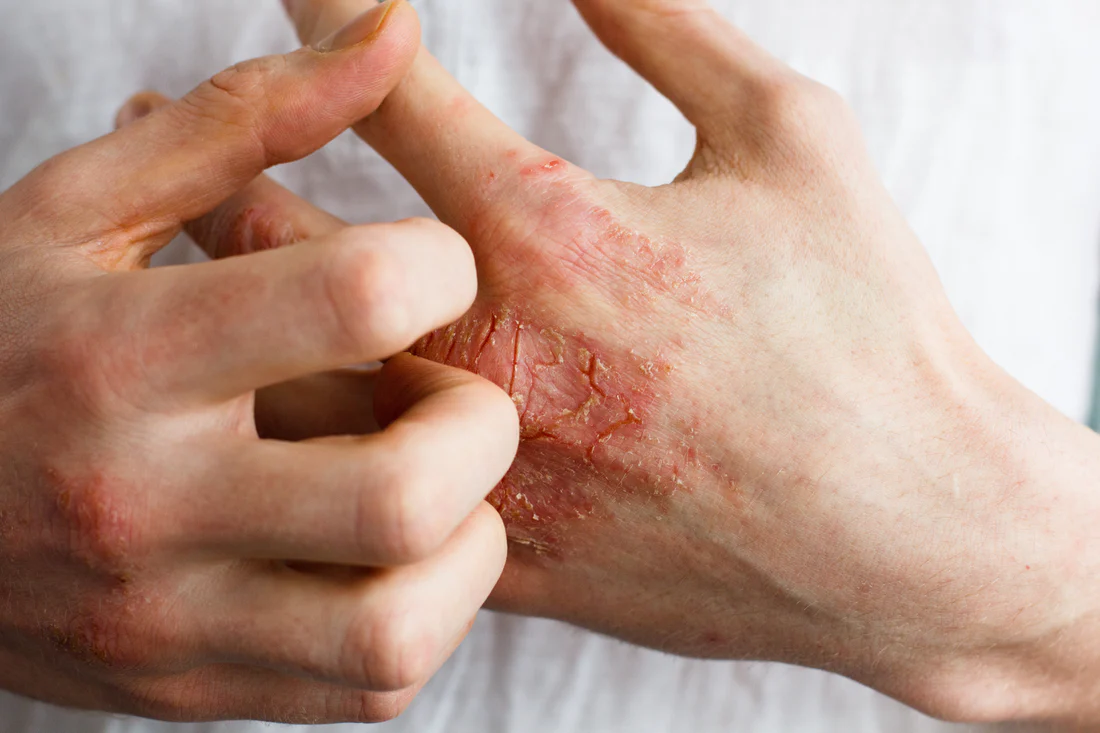
Quick snapshot: scabies vs eczema
| Clue | More like scabies | More like eczema |
|---|---|---|
| Itch timing | Intense, often worse at night | Itchy off and on, often worse with dry air, heat, sweat, or after bathing |
| Spread | Often spreads to close contacts, siblings, caregivers | Does not spread person-to-person |
| Contagious? | Yes, mainly by prolonged skin-to-skin contact; sometimes via shared bedding/clothing (risk is higher in crusted scabies) | No |
| Pattern | Small bumps, clusters, scratch marks; may see thin “burrows” | Dry, rough patches; red, inflamed areas; may ooze or crust if infected |
| Common locations | Between fingers, wrists, elbows, armpits, waistline, groin, buttocks; in babies also scalp, face, palms, soles | Babies: cheeks/scalp/extensors; older kids: inside elbows, behind knees, neck, wrists, ankles |
If your child has eczema, they can still catch scabies. So if something suddenly looks “different” than their usual flare, trust your gut and look for the scabies clues below.
What scabies looks like in kids
Scabies is caused by a tiny mite that burrows into the top layer of skin. The rash is partly from the mite and partly from your child’s immune reaction to it.
Common scabies signs
- Very itchy rash, often worse at night (families often tell me bedtime becomes a scratching marathon).
- Small red bumps that can look like pimples, bug bites, or tiny hives.
- Scratch marks and crusting from constant itching.
- Burrows: thin, slightly raised, wavy or straight lines in the skin. They can be subtle, especially on squirmy kids and on darker skin tones.
Where it shows up: between the fingers, wrists, elbows, armpits, belly button area, waistline, buttocks, and groin. In babies and toddlers, scabies can also involve the scalp, neck, face, palms, and soles. In older children and adults, face and scalp involvement is uncommon.
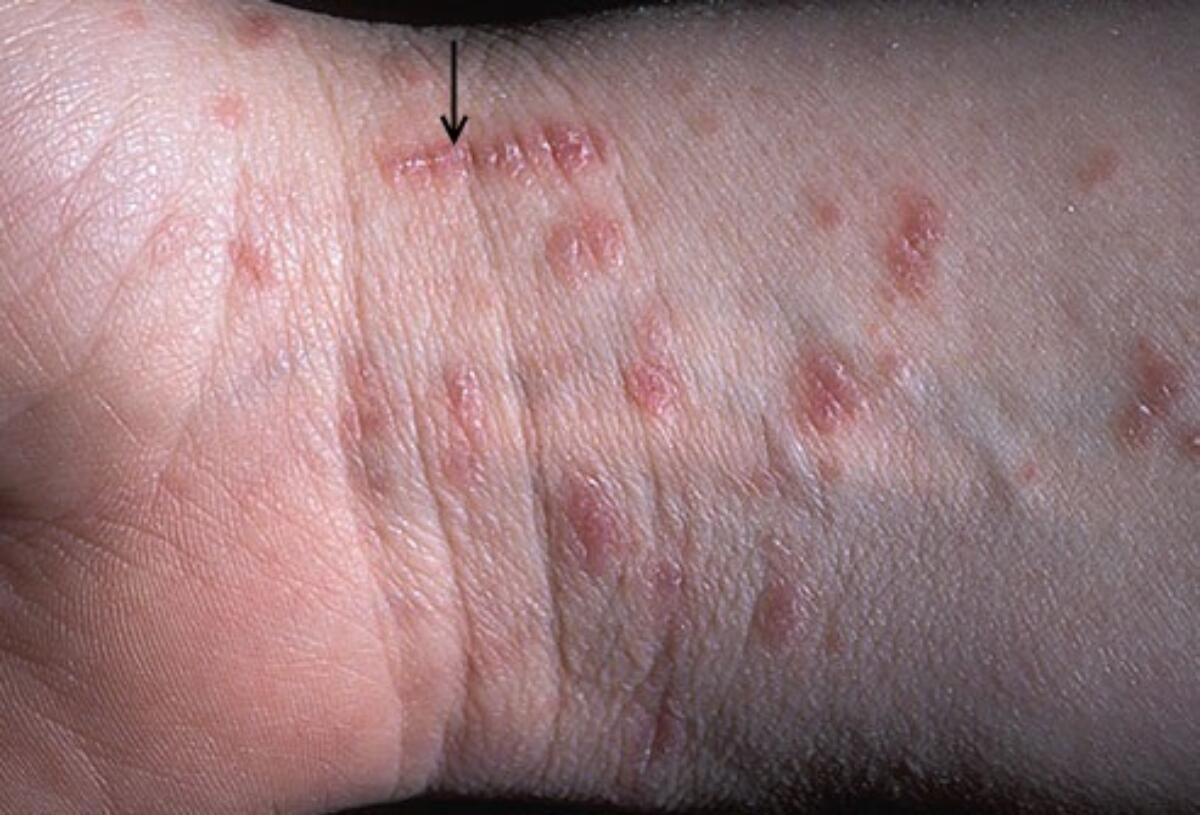
What eczema looks like in kids
Eczema, also called atopic dermatitis, is a chronic tendency toward dry, inflamed, easily irritated skin. It tends to flare with triggers like dry weather, hot baths, fragranced products, sweat, illness, and stress.
Common eczema signs
- Dry, rough, or scaly patches.
- Redness that can look pink, red, purple, gray, or ashy depending on skin tone.
- Thickened skin in spots that get rubbed or scratched a lot (especially in older kids).
- Oozing or crusting can happen, usually from irritation or secondary infection, not from “mites.”
Where it shows up: in babies often on the cheeks and scalp, and on the outer arms and legs. In older children it commonly settles into the “creases” like inside the elbows and behind the knees, plus wrists, ankles, and neck.
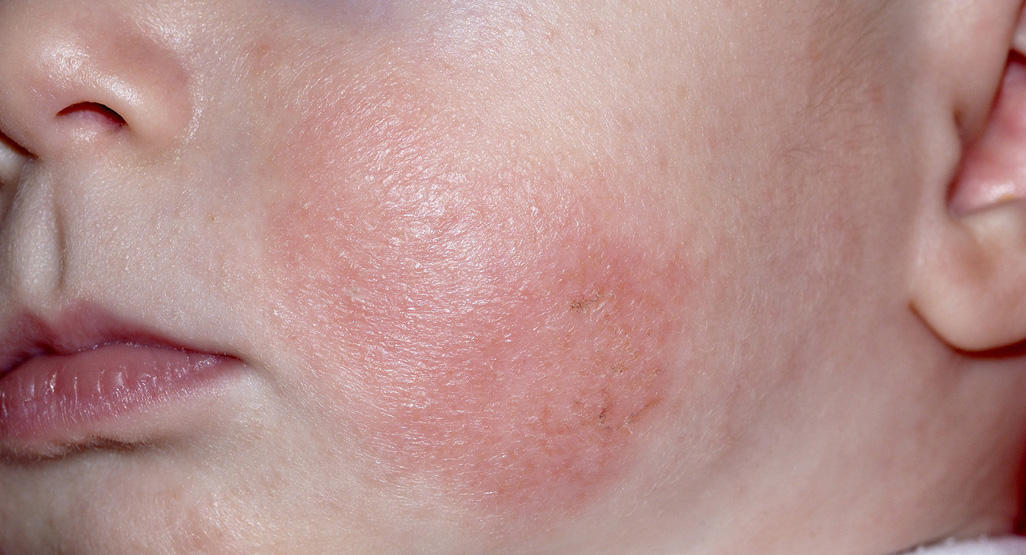
The pattern clue
If you remember one thing from this article, make it this section.
Scabies pattern
- Clusters of small bumps and lots of scratch marks.
- Possible burrows: thin, slightly raised lines that can look like a faint pencil mark under the skin.
- Household pattern: more than one person itching, or a new itch after a sleepover, travel, shared bedding, or close contact.
Eczema pattern
- Dry “map-like” patches that come and go.
- Symmetry is common: both wrists, both elbow creases, both behind-knee areas.
- Trigger pattern: flare after a new soap, bubble bath, detergent, swimming, seasonal change, or sweating.
The timing clue
Scabies itch is famously worse at night. Kids can be distracted during the day, then the itch ramps up when they settle down. You might also notice your child waking more often and needing help not to scratch.
Eczema itch can be worse at night too, especially when skin is dry and warm under pajamas. The difference is the overall story: eczema usually has a known history of dry, sensitive skin and flares with triggers, while scabies often has a sudden, intense itch and a “this is spreading” feeling in close contacts.
Spread and contagiousness
Scabies is contagious. It spreads mainly through prolonged skin-to-skin contact. It can sometimes spread through shared clothing, towels, and bedding, and that risk is higher with crusted scabies (a more severe form with a very high mite burden).
Eczema is not contagious. Your child cannot “give” eczema to anyone else.
If more than one household member is itching, or your child’s school or daycare mentions scabies, move scabies higher on your list.
How scabies is diagnosed
Often, scabies is diagnosed by a clinician based on the story (night itch, contact exposure) and a close look at the rash distribution. Sometimes they use dermoscopy (a special magnifier) to look for mites or burrows, or they may do a skin scraping to confirm under a microscope.
Clear photos taken in good light can be very helpful, especially if the rash changes from hour to hour or your child is not in the mood to “hold still for science.”
When you can treat at home and when you should call
Home care is reasonable for a typical eczema flare
If your child has a known eczema pattern and they feel otherwise well, you can usually start with basic flare care:
- Moisturize twice daily with a thick, fragrance-free ointment or cream.
- Short, lukewarm baths, then moisturize within a few minutes of getting out.
- Use fragrance-free soap and detergent.
- Topical steroid: if your pediatrician has prescribed one before for flares, use it exactly as directed.
If it is not improving in a few days, is disrupting sleep, or is happening frequently, check in with your child’s pediatrician. You may need a tailored plan or a different medication.
Call your child’s pediatrician promptly if scabies is likely
Scabies usually needs prescription treatment. Over-the-counter itch creams will not eradicate mites.
- Ask about permethrin 5% cream, which is a common first-line treatment for kids in many settings.
- Many treatment plans use two applications (for example, one now and a repeat about 7 days later), because the second round helps catch newly hatched mites.
- Close contacts usually need treatment at the same time, even if they are not itchy yet, because symptoms can take weeks to show up after first exposure.
- Your clinician may also discuss oral ivermectin in certain cases (like outbreaks, crusted scabies, or treatment-resistant cases). It is not used for all ages and weights, and it is generally avoided in pregnancy. Your clinician will guide you on whether it is appropriate.
Common permethrin details parents ask about: it is typically applied to the whole body from the neck down and left on for 8 to 14 hours before washing off. In infants and toddlers, clinicians often include the scalp, hairline, neck, and ears because scabies can show up there. Follow the exact instructions you are given, since age and local guidance matter.
While you are waiting to be seen, focus on itch control and reducing scratching to protect your child’s skin barrier.
What not to use
When parents are desperate, they understandably reach for anything that promises relief. A few things I recommend avoiding:
- Do not use “scabies home remedies” like bleach, kerosene, gasoline, or harsh disinfectants on skin. These can cause chemical burns and do not safely treat scabies.
- Do not use essential oils as a primary treatment for suspected scabies. They can irritate skin, especially eczema-prone skin, and they are not a reliable eradication plan.
- Do not overuse topical steroid creams on a rash that could be scabies. Steroids can calm redness and itching temporarily, which may delay diagnosis while mites keep spreading.
- Do not use topical numbing products (like benzocaine) on young children unless directed by a clinician. Some can cause serious side effects.
- Avoid fragranced lotions and bubble baths, especially if eczema is on the table.
How to reduce itch safely while you wait
- Cool compresses for 5 to 10 minutes on itchy spots.
- Keep nails short. For little kids, consider cotton mittens at night if scratching is intense.
- Loose, breathable pajamas.
- Ask your pediatrician about an age-appropriate antihistamine for nighttime itch. Some are better for allergies than skin itch, but they can help certain kids sleep.
- Moisturize even if you suspect scabies. Scratching damages the skin and moisturizer helps protect that barrier.
If scabies is suspected: cleaning that matters
This is where parents often go into full deep-clean mode. You do not need to disinfect your entire home from top to bottom.
Focus on items used in the last 72 hours
- Wash bedding, pajamas, and recently worn clothes used in the past 3 days (72 hours) in hot water and dry on high heat.
- Items you cannot wash can be sealed in a bag for at least 3 days (some guidance suggests longer, like up to a week). Follow your clinician or public health instructions.
- Vacuum soft surfaces if you want to, but the highest value is treating people correctly and laundering linens and clothing.
Most treatment failures I saw in clinic were not from “not bleaching the couch.” They were from missing a close contact, applying medication incorrectly, or not doing treatments at the same time.

Crusted scabies
Crusted scabies is uncommon, but important. It can happen in people with weakened immune systems or certain neurologic conditions, and it is highly contagious. The skin may look thick, scaly, or crusted, and itch can be variable. If you think this is a possibility, seek prompt medical care because treatment and cleaning recommendations are more intensive.
Common look-alikes
Because parenting is never simple, a few other conditions can imitate scabies or eczema:
- Bug bites (often in exposed areas, may appear in lines or clusters after sleep).
- Contact dermatitis (reaction to a new soap, lotion, plant, metal, or detergent, usually where the skin touched the trigger).
- Impetigo (honey-colored crusting, can occur on top of eczema or scratching).
- Hand-foot-and-mouth disease (mouth sores plus rash on palms/soles, often with fever).
- Ringworm (round, scaly patch with a clearer center).
If you are not sure, it is absolutely appropriate to send photos to your pediatrician’s portal or book a visit. Getting it right early saves a lot of sleep later.
Return to school or daycare
Policies vary, but many schools and daycares allow children with scabies to return after the first treatment, as long as treatment has started. Ask your pediatrician and follow your school or daycare guidance. It is also wise to notify close contacts so other families can watch for symptoms and get treated if needed.
Urgent care and ER triggers
Most itchy rashes are not emergencies, but some situations should be evaluated quickly.
Get same-day care if:
- Your child has fever plus a new rash, especially if they seem ill.
- The skin looks infected: increasing redness, warmth, swelling, pain, pus, honey-colored crusts, or red streaks.
- Your child is a newborn or very young infant with a widespread rash.
- Your child has severe eczema with painful, rapidly spreading areas or blisters.
- Your child has significant itch with sleep disruption for multiple nights and the rash is spreading.
Go to the ER now if:
- There are signs of a severe allergic reaction: trouble breathing, swelling of lips or face, widespread hives with vomiting, or fainting.
- Your child is very lethargic, difficult to wake, or you are worried about dehydration.
- The rash includes purple or bruise-like spots that do not blanch (do not fade when pressed), especially with fever.
- You suspect eczema herpeticum: clusters of painful blisters or punched-out sores, fever, and a child who seems unwell, particularly if they have eczema and possible exposure to cold sores.
Questions parents ask
Can eczema suddenly start looking like scabies?
Eczema can flare hard and look bumpy, especially if your child scratches a lot. But new intense nighttime itching, bumps in the finger webs or wrists, and other family members itching are the scabies clues that make me pause.
Can my child have both?
Yes. Kids with eczema have a weaker skin barrier, which can make them more sensitive to irritation and more likely to get secondary infections. They can also catch scabies like anyone else.
If we treat scabies, how fast does itching stop?
Even after successful treatment, itching can persist for 2 to 4 weeks (sometimes longer) because the skin is still reacting. You may hear this called post-scabetic itch, and some children get lingering itchy nodules. That does not always mean treatment failed. If itching is not improving, new bumps keep appearing, or others in the home develop symptoms, check back with your pediatrician.
A calm next step
If you suspect eczema, start gentle skin care and see how your child responds over the next couple of days. If you suspect scabies, focus on getting a prompt diagnosis, treating close contacts at the same time, and laundering items used in the last 72 hours.
And if you are stuck in the gray zone, take a few clear photos in good light and call your pediatrician. You do not need to solve this alone at 3 AM. That is my job.