Scalp Ringworm (Tinea Capitis) in Kids
Sarah Mitchell
Sarah Mitchell is a Registered Pediatric Nurse and a mother of three who has spent over a decade helping families navigate the beautiful, chaotic early years of childhood. She combines evidence-based medical knowledge with real-world parenting experience to offer practical, compassionate advice. At Awesome Parent, Sarah's mission is to help exhausted parents find solutions, trust their instincts, and finally get some sleep.
If you are staring at a flaky patch on your child’s scalp and thinking, Is this just dandruff or is my kid losing hair? you are not being dramatic. One common reason kids develop scaly spots with broken hairs or patchy hair loss is tinea capitis, also known as scalp ringworm.
Despite the name, it is not a worm. It is a fungal infection that likes warm, slightly sweaty places and spreads easily in kid-world: close play, shared hats, sleepovers, sports helmets, and the magical black hole known as the classroom dress up bin.
This page focuses on tinea capitis specifically. If you want the big picture on ringworm on the body, check our general ringworm guide on Awesome Parent.
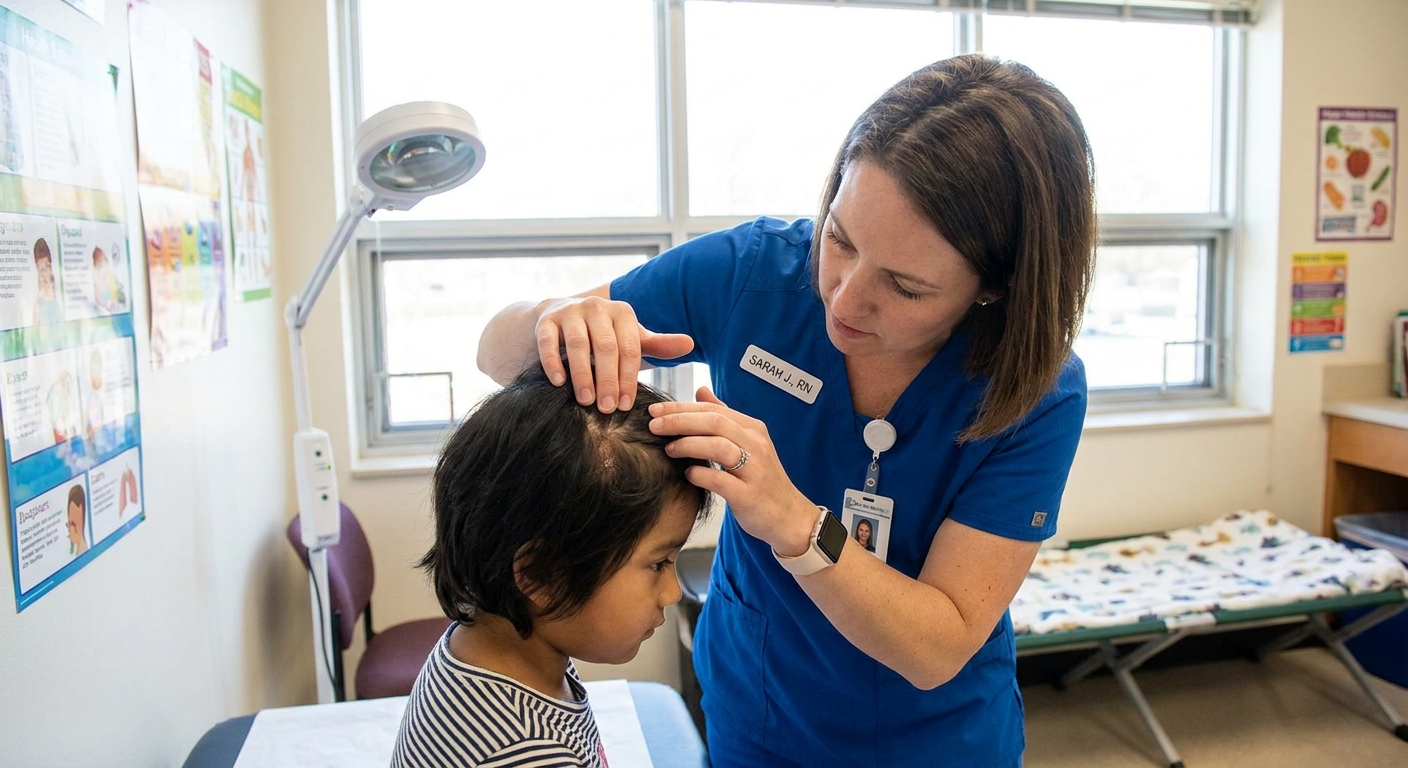
What scalp ringworm looks like
Tinea capitis can be sneaky. Some kids have obvious round patches. Others look like they just need a better shampoo. The clues are in the hair and the edges of the patch.
Common signs parents notice
- Flaky, scaly patches on the scalp that do not clear with normal washing
- Broken hairs that look like black dots or short stubble in a patch
- Patchy hair loss or thinning, often with scale
- Itching (sometimes intense, sometimes barely there)
- Redness or mild swelling around the patch
- Swollen lymph nodes behind the ears or at the back of the neck
Some kids develop a more inflamed, tender, boggy area called a kerion. It can ooze, crust, or look like a painful lump. This can be mistaken for a bacterial infection, but it is often still fungus at the root of the problem.
Important: Tinea capitis can be present even if there is no perfect “ring” shape. On the scalp, it often shows up as irregular patches with scaling and broken hairs.
Ringworm vs cradle cap vs dandruff
This is the part that makes parents feel like they are failing a pop quiz at 2 AM. The good news is you are not expected to diagnose skin conditions from across the room. Here are the most useful differences to know.
Cradle cap
- Most common in babies, especially under 12 months
- Looks like greasy yellow or white scale that can be thick
- Usually not associated with true patchy hair loss
- Often shows up on eyebrows, behind ears, or diaper area too
- Usually improves gradually with gentle scalp care
Dandruff
- More common after puberty, but can happen earlier
- Looks like diffuse flaking across the scalp, not one expanding patch
- Hair typically stays intact
- May be worse in winter or with certain hair products
Tinea capitis
- Most common in preschool and elementary-aged kids
- Often has one or more patches that spread or multiply
- Broken hairs, black-dot stubble, or patchy hair loss are big clues
- May have itching and sometimes tender bumps
- Often does not respond to typical dandruff or cradle cap routines
If you are deciding whether to call the pediatrician, I use this simple rule: Flakes plus broken hairs or a bald patch equals “get it checked.”

How kids catch it
Tinea capitis spreads through direct contact and shared items. The fungus can live on hair shafts and skin cells, and those can travel farther than you would think on everyday kid gear.
Common ways it spreads
- Head-to-head contact during play
- Shared hats, helmets, hoods, and hair accessories
- Shared hairbrushes, combs, clips, barrettes
- Pillows, blankets, towels especially in shared bedding situations
- Barbershops or salons with poorly disinfected tools (less common, but possible)
- Pets like kittens and cats can carry certain fungi, sometimes with subtle or no symptoms
Here is the frustrating part: a child can carry the fungus with minimal symptoms at first, and by the time the first patch is obvious, it may have already moved through siblings or classmates.
Home steps that help
These steps can lower spread and reduce the chance of ping-pong reinfection. They do not replace medical treatment.
- Assign your child their own brush, comb, hair ties, hats, and pillow while treating.
- Soak combs and brushes in hot soapy water and then disinfect per product guidance (keep cleaners safely out of reach).
- Wash pillowcases, hats, and bedding in hot water if possible and dry thoroughly.
- Do not share sports helmets, or wipe the inside per team policy.
- Check other kids in the home for itching, flakes, or small patches.
Highest-yield tip: stop sharing hair tools and headwear. That single change matters more than most elaborate cleaning plans.
Why OTC shampoos fail
This is where a lot of good, attentive parents get stuck. They try dandruff shampoo, baby oil, a scalp brush, maybe even a “natural antifungal” from the internet. And the patch keeps spreading.
The main reason is simple: tinea capitis usually requires prescription oral medication because the fungus infects the hair shaft and follicles. Shampoos alone do not reliably penetrate deep enough to clear it.
Are antifungal shampoos useless?
Not useless. They can help reduce shedding of spores and lower transmission risk, especially early on or alongside oral treatment. Clinicians often recommend antifungal shampoos such as ketoconazole or selenium sulfide as an add-on, typically a few times per week.
In some practices, household members (even if they have no symptoms) may also be advised to use an antifungal shampoo for a short period to reduce spread. Your clinician can tell you what they recommend for your situation.
But if you are only using over-the-counter scalp care and your child has broken hairs or a bald patch, it is very common for the infection to persist until the inside-out treatment is started.
What clinicians look for
In clinic, we think about three things: Is this really tinea capitis? How inflamed is it? and how do we stop it from spreading?
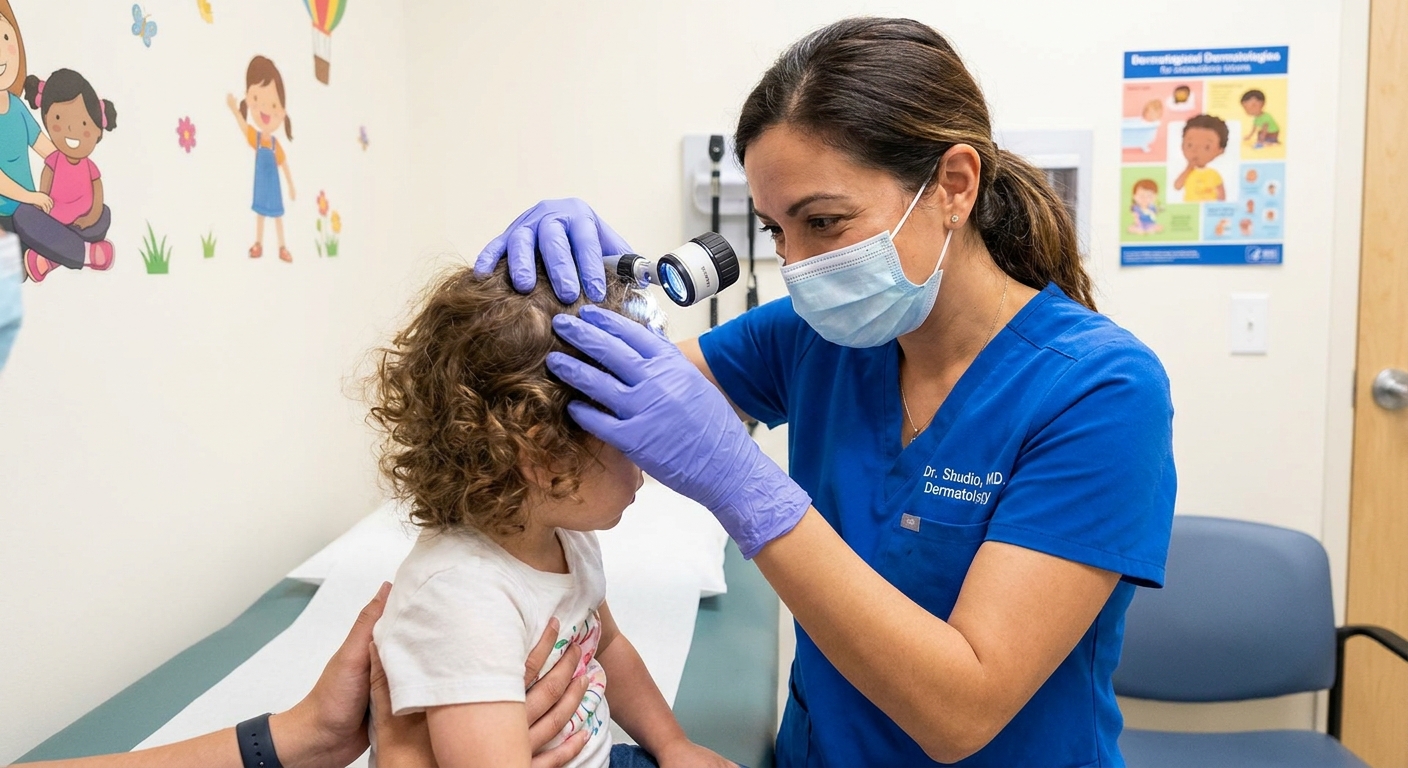
How it is diagnosed
- Scalp and hair exam with good lighting and a careful look for broken hairs
- Sometimes a fungal culture or PCR test from scalp scrapings or hairs to identify the organism (results can take time)
- In some offices, a special light called a Wood’s lamp may be used. Fluorescence is more typical of some Microsporum species and is uncommon with many Trichophyton infections, so a normal result does not rule it out.
Treatment basics
Most cases need:
- Oral antifungal medication for several weeks (the exact choice depends on your child’s age, health history, and what organism is suspected)
- Antifungal shampoo a few times weekly to reduce spread
- Family and close contact guidance to prevent reinfection
You may hear common first-line options like griseofulvin or terbinafine. Which one is best can depend on the likely fungus in your area (and sometimes culture results), plus your child’s age and medical history. Your clinician will pick what fits.
How long it takes
Many kids need treatment in the range of 6 to 8 weeks, sometimes longer depending on the medication and the organism. Symptoms often start to look better before the fungus is fully cleared, so finishing the course matters. Follow-up may include a recheck exam, and sometimes repeat testing if it is not improving as expected.
If there is a kerion (the boggy, tender kind), clinicians may treat more aggressively. In select cases, they may add other medications to calm inflammation and protect hair regrowth.
Hair usually grows back, but it can take time. The earlier it is treated, the better the odds of avoiding scarring or prolonged shedding.
School and daycare
This is a common stress point, because nobody wants the “your child is contagious” phone call.
Many schools and daycares allow return once treatment is started, but policies vary, so check with your setting.
Even after starting treatment, the fungus may still be present for a bit. That is why not sharing hats or brushes, and using the recommended shampoo, really matters.
Call the doctor sooner
Call your child’s provider if you notice:
- A bald patch or expanding area of hair thinning
- Broken hairs or black-dot stubble
- Painful swelling, pus, crusting, or a boggy lump (possible kerion)
- Fever or your child seems unwell
- Swollen lymph nodes plus a scalp rash
- A newborn or medically fragile child in the home and you are worried about spread
If your child is scratching enough to break the skin, that can open the door to a secondary bacterial infection. That is another good reason to get eyes on it promptly.
Comfort tips while you wait
Waiting for an appointment while your child scratches is its own special kind of torture. A few safe comfort measures:
- Keep nails short to reduce skin damage from scratching.
- Use a gentle fragrance-free shampoo on non-treatment days.
- A cool washcloth on itchy areas can help.
- Try to avoid heavy oils or thick product buildup that can make the scalp harder to evaluate.
Skip steroid creams on the scalp unless a clinician recommends them. Steroids can temporarily reduce redness and itching while allowing fungal infections to quietly worsen.
Pets and ringworm
If you have a new kitten, a cat with patchy fur, or a pet with suspicious skin spots, mention it to your child’s clinician. Sometimes the best next step is also a quick call to your veterinarian, since pets can be a source (and can keep the cycle going if untreated).
Quick recap
- Scalp ringworm often looks like flakes plus broken hairs or patchy hair loss.
- It spreads through head contact and shared items like hats, helmets, brushes, and bedding.
- Over-the-counter dandruff care often fails because tinea capitis usually needs oral prescription treatment.
- Get medical advice quickly if there is a tender, swollen, oozing area or significant hair loss.
Parenting note from a pediatric nurse mom: if your gut is telling you “this is not just dandruff,” you are probably right. You do not need to wait until the patch gets bigger to ask for help.
Medical disclaimer
This article is for general education and does not replace medical care. If you think your child may have scalp ringworm or any rapidly worsening rash, contact your pediatrician or a dermatologist for diagnosis and treatment.