Scarlet Fever in Kids: Rash, Symptoms, and Treatment
Sarah Mitchell
Sarah Mitchell is a Registered Pediatric Nurse and a mother of three who has spent over a decade helping families navigate the beautiful, chaotic early years of childhood. She combines evidence-based medical knowledge with real-world parenting experience to offer practical, compassionate advice. At Awesome Parent, Sarah's mission is to help exhausted parents find solutions, trust their instincts, and finally get some sleep.
If your child has a sore throat and then suddenly breaks out in a rough, red rash, it is completely normal to feel alarmed. The good news is that scarlet fever is treatable and, in most cases, kids bounce back quickly once they start the right antibiotic.
Scarlet fever is not a separate “mystery illness.” It is a Group A strep infection (the same bacteria that causes strep throat) where certain strains release pyrogenic (erythrogenic) exotoxins that trigger a classic rash. Let’s walk through what to look for, what to do, and what other rashes can look similar.
What is scarlet fever?
Scarlet fever is an infection caused by Group A Streptococcus (often called “Group A strep” or just “strep”). Some strains make toxins that lead to the signature sandpaper-like rash.
Most kids with scarlet fever also have symptoms of strep throat, though it can also happen with other strep infections (like skin infections) in rare cases.
- It is contagious. It spreads mainly through respiratory droplets (coughing, sneezing, sharing drinks or utensils).
- It is treatable. Antibiotics shorten the illness, reduce spread, and help prevent complications.
- It is not caused by a virus. That matters because viral rashes are common, and antibiotics will not help those.
How it spreads and timing
After exposure to Group A strep, symptoms often show up in about 2 to 5 days.
In many kids, the sore throat and fever start first, and the rash follows about 12 to 48 hours later. It is not a rule, but it is a common pattern.
Symptoms to watch for
Kids can look different from one another, but scarlet fever has a pretty recognizable pattern. Often, the sore throat and fever show up first, followed by the rash within about a day or two.
Common symptoms
- Fever (often 101°F to 104°F)
- Sore throat and pain with swallowing
- Red, swollen tonsils, sometimes with white patches or streaks of pus
- Swollen, tender neck glands
- Headache
- Stomach pain, nausea, or vomiting (yes, strep can do this)
- Fatigue and feeling run-down
Classic clues
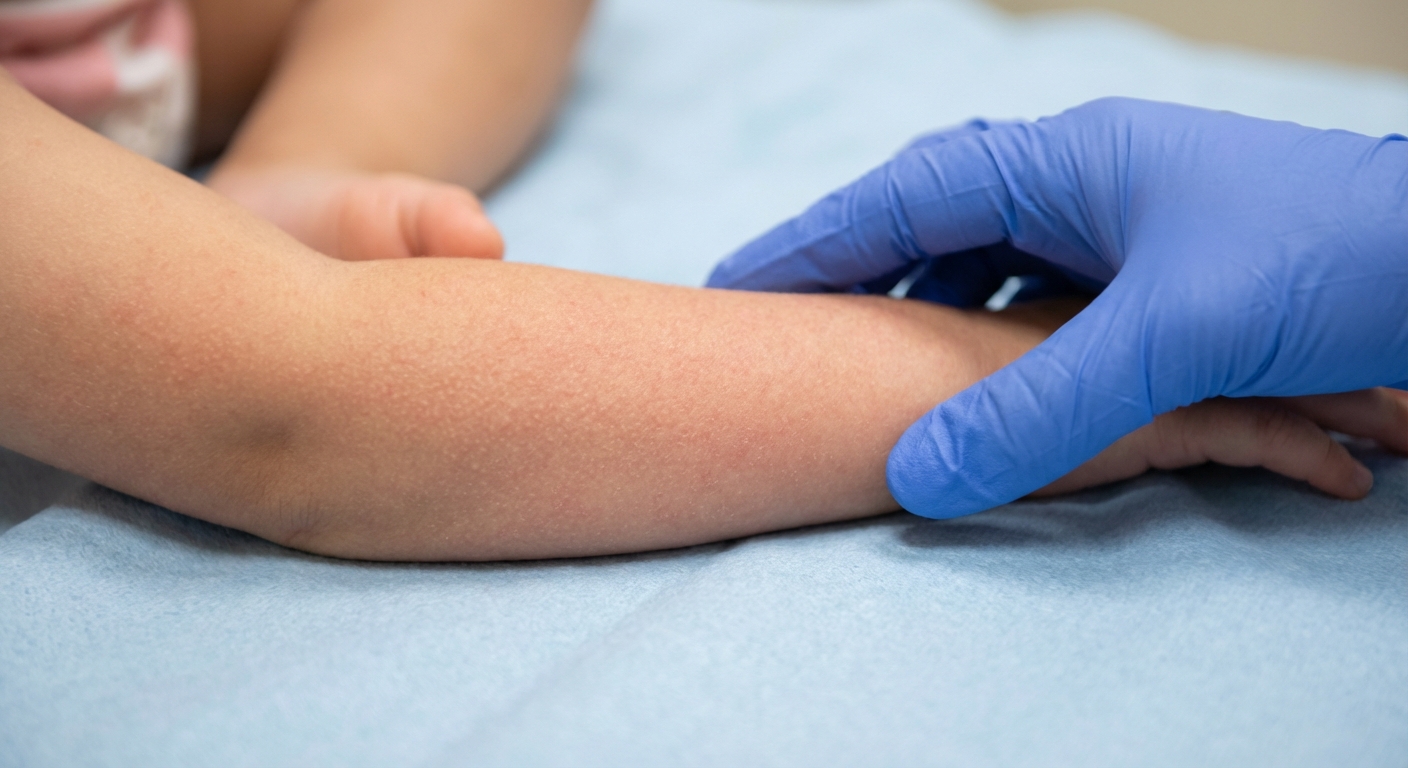
The rash: Scarlet fever’s rash is usually fine, red, and rough, often described as feeling like sandpaper. It can look like a sunburn with tiny bumps.
- Often starts on the chest, neck, or upper back, then spreads to the trunk and limbs
- May be more noticeable in skin folds like the armpits, elbows, and groin (often called Pastia’s lines)
- Can cause flushed cheeks with a paler area around the mouth (circumoral pallor)
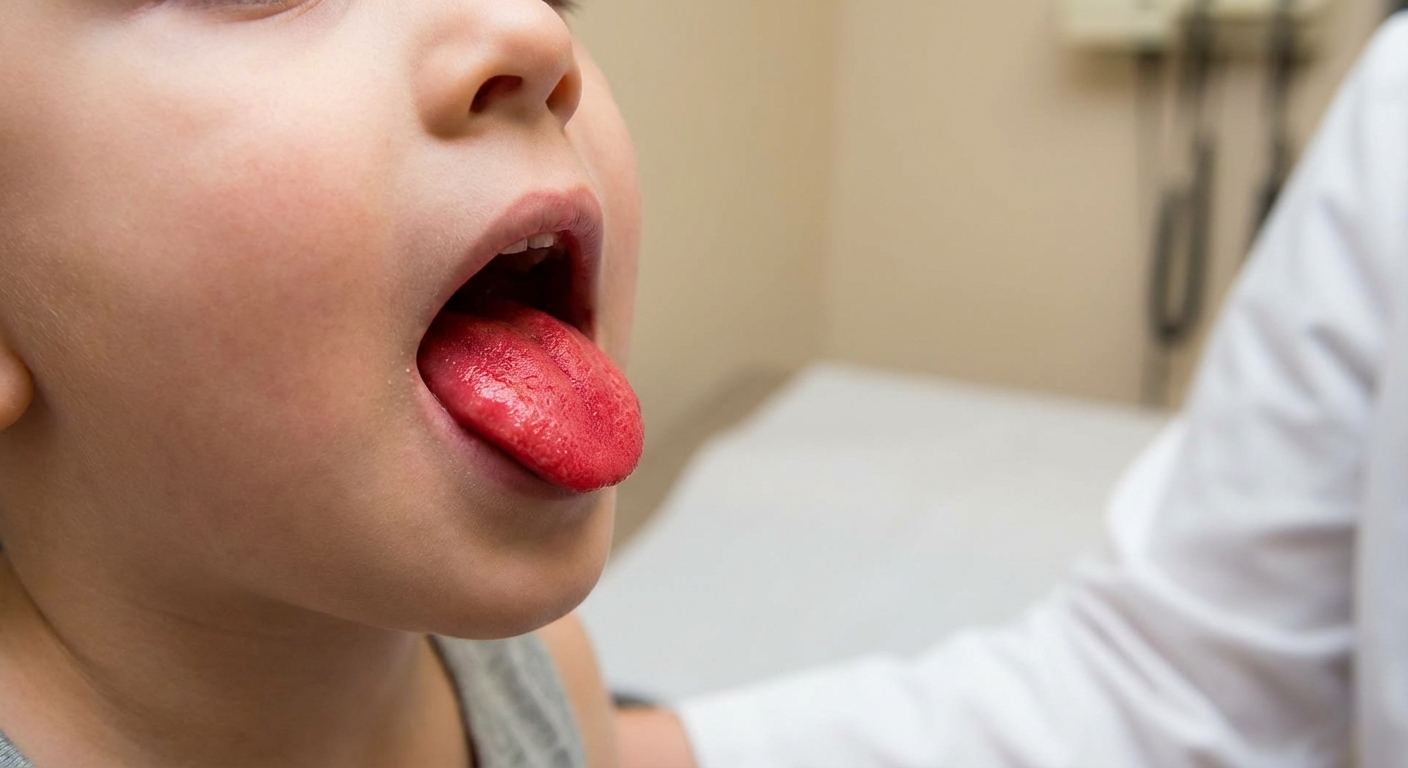
Strawberry tongue: The tongue may look bright red with prominent bumps. Sometimes it starts with a whitish coating that sloughs off, leaving the red “strawberry” look.
A note about darker skin tones: On deeper skin tones, the redness of the rash may be subtler. The texture (that sandpaper feel), swelling, warmth, and the pattern of symptoms (fever plus sore throat) can be more helpful clues than color alone.
How it is linked to strep
Scarlet fever is essentially strep infection plus rash. If your child has the rash, the most common source is strep throat.
Clinicians typically confirm strep with:
- Rapid strep test (results in minutes)
- Throat culture if the rapid test is negative but suspicion stays high (results in 1 to 2 days)
On exam, providers may also look for things like tender anterior cervical lymph nodes, tonsillar swelling or exudate, and the rash’s sandpaper texture, especially in skin folds.
One helpful nuance: When classic viral symptoms dominate (cough, runny nose, hoarseness, oral ulcers), strep testing is often less likely to be useful. Your clinician will guide you, especially if local outbreaks or exposures change the odds.
Treatment
The correct treatment for scarlet fever is an antibiotic that targets Group A strep. This does three important jobs: it helps your child feel better faster, reduces contagiousness, and helps prevent certain complications.
Antibiotics
Common options include:
- Penicillin or amoxicillin (most common first choices)
- If your child has a penicillin allergy, providers may use other options like cephalexin (often avoided in immediate-type allergy such as anaphylaxis) or azithromycin, depending on the allergy history and local resistance patterns
Important: Even if your child looks better after a day or two, it is still important to finish the full course exactly as prescribed.
Also important: Do not use leftover antibiotics and do not share antibiotics between kids. The right drug and dose matters, and using the wrong antibiotic can delay care and increase resistance.
How fast kids improve
- Fever and throat pain often improve within 24 to 48 hours after starting antibiotics.
- The rash can take a bit longer to fade. As it resolves, some kids have peeling skin, especially on the fingertips, toes, or groin area. That can look dramatic and still be part of normal recovery.
Comfort care at home
- Fluids (cold drinks, smoothies, popsicles)
- Soft foods (yogurt, soup, applesauce)
- Acetaminophen or ibuprofen for pain and fever if your child can take them safely based on age and medical history
- Humidifier and warm showers for throat comfort
- Replace toothbrush after 24 hours on antibiotics (not strictly required, but it is a simple step many families like)
A quick safety note: avoid aspirin in children due to the risk of Reye syndrome.
How long is it contagious?
Without antibiotics, people with strep can remain contagious for a while, often around 2 to 3 weeks in some cases. With appropriate antibiotics, most kids are considered much less contagious after:
- At least 24 hours on antibiotics and
- Fever-free for 24 hours without fever-reducing medicine
In practical terms: many schools and daycares allow return after 24 hours of antibiotics plus being fever-free and improving. When in doubt, follow your child’s school policy and your clinician’s guidance.
When to call the doctor
If you suspect scarlet fever, it is worth calling your child’s pediatrician the same day, especially if there is a sore throat and fever along with the rash. Strep needs antibiotics, and it is not something you want to “wait out” if the signs fit.
Call soon if your child has
- Sore throat with fever and a new rough red rash
- Known strep exposure plus symptoms
- Rash that is spreading quickly or causing significant discomfort
- Symptoms that are not improving after 48 hours on antibiotics
Go urgently if your child has
- Trouble breathing, drooling, or cannot swallow saliva
- Signs of dehydration (very little urine, dry mouth, no tears, lethargy)
- Severe headache with stiff neck, confusion, or extreme sleepiness
- A rash with blistering, significant skin pain, or purple bruising-like spots
- Any signs of a serious allergic reaction after starting medication (hives, swelling of lips or face, wheezing)
Possible complications
Most kids do very well with treatment. The reason clinicians take strep and scarlet fever seriously is that untreated Group A strep can lead to complications.
What can happen
- Acute rheumatic fever (can affect the heart, joints, and nervous system). Antibiotics help prevent this.
- Post-streptococcal glomerulonephritis (a kidney inflammation that can happen after strep infections). Antibiotics do not reliably prevent this, but treatment is still important for symptom improvement and reducing spread.
- Ear infections or sinus infections
- Peritonsillar abscess (a painful collection near the tonsil)
- Spread of infection to other areas in rare cases
This is why getting evaluated and treated matters, even if your child is trying to tough it out.
Scarlet fever vs other rashes
Rashes are one of the most common reasons parents call the clinic, and I get it. They can all look the same at 2 AM under hallway lighting. Here are a few ways scarlet fever often differs from other common rashes.
Viral rash
- Scarlet fever: often comes with sore throat, fever, and a rough, sandpaper texture.
- Viral rashes: often come with cough, runny nose, hoarseness, and the rash is usually smoother and less sandpapery.
Hand, foot, and mouth
- Hand, foot, and mouth: commonly causes small blisters on hands and feet and painful mouth sores.
- Scarlet fever: more likely to cause a diffuse fine rash on the trunk and a prominent sore throat.
Allergic rash (hives)
- Hives: raised, itchy welts that move around and change shape quickly.
- Scarlet fever: a more uniform rash that does not typically migrate like hives.
Eczema flare
- Eczema: usually chronic, very itchy patches in typical areas (behind knees, inside elbows), often with known triggers.
- Scarlet fever: sudden onset with fever and throat symptoms, plus the sandpaper feel.
If the rash is accompanied by a sore throat and fever, it is worth thinking “strep until proven otherwise,” and getting tested.

Can it happen again?
Yes. Immunity is not guaranteed, and kids can get strep multiple times. If your child has had scarlet fever before and develops similar symptoms again, it is still worth testing rather than assuming it is the same illness repeating.
Frequently asked questions
Does it always cause a rash?
No. Many kids get strep without developing the rash. Scarlet fever is the subset where the toxin triggers the rash.
Will the rash go away on its own?
The rash will fade, but scarlet fever is still a strep infection. Treating with antibiotics is important to reduce contagiousness and help prevent complications like acute rheumatic fever.
Can my child go to school with the rash?
Typically, kids can return after 24 hours of antibiotics and when they are fever-free for 24 hours (without fever-reducing medicine) and feeling well enough to participate. The rash itself may linger longer, and that is okay.
The calm takeaway
If you are seeing a sandpaper-like rash along with fever and a sore throat or “strawberry tongue,” scarlet fever is a strong possibility. It is scary-looking, but it is also one of those illnesses where getting the right test and the right antibiotic can make a big difference quickly.
When you call your pediatrician, it helps to mention: the timing of fever, when the rash started, whether your child has throat pain, and any known strep exposure. You are not overreacting. You are paying attention, and that is exactly what your kid needs.