Shingles in Children
Sarah Mitchell
Sarah Mitchell is a Registered Pediatric Nurse and a mother of three who has spent over a decade helping families navigate the beautiful, chaotic early years of childhood. She combines evidence-based medical knowledge with real-world parenting experience to offer practical, compassionate advice. At Awesome Parent, Sarah's mission is to help exhausted parents find solutions, trust their instincts, and finally get some sleep.
If you have ever seen shingles in an adult, the idea of it showing up on your child can feel unfair and a little alarming. The good news is that shingles in children is usually milder than in adults, and most kids recover without problems. The tricky part is recognizing it early, keeping your child comfortable, and knowing when they can be around other people.
This guide is for general education and is not a substitute for medical care. If you are worried, call your child’s clinician.
Let us walk through what shingles is, what the rash typically looks like, how to handle pain and itching at home, and the situations where you should call your pediatrician the same day.
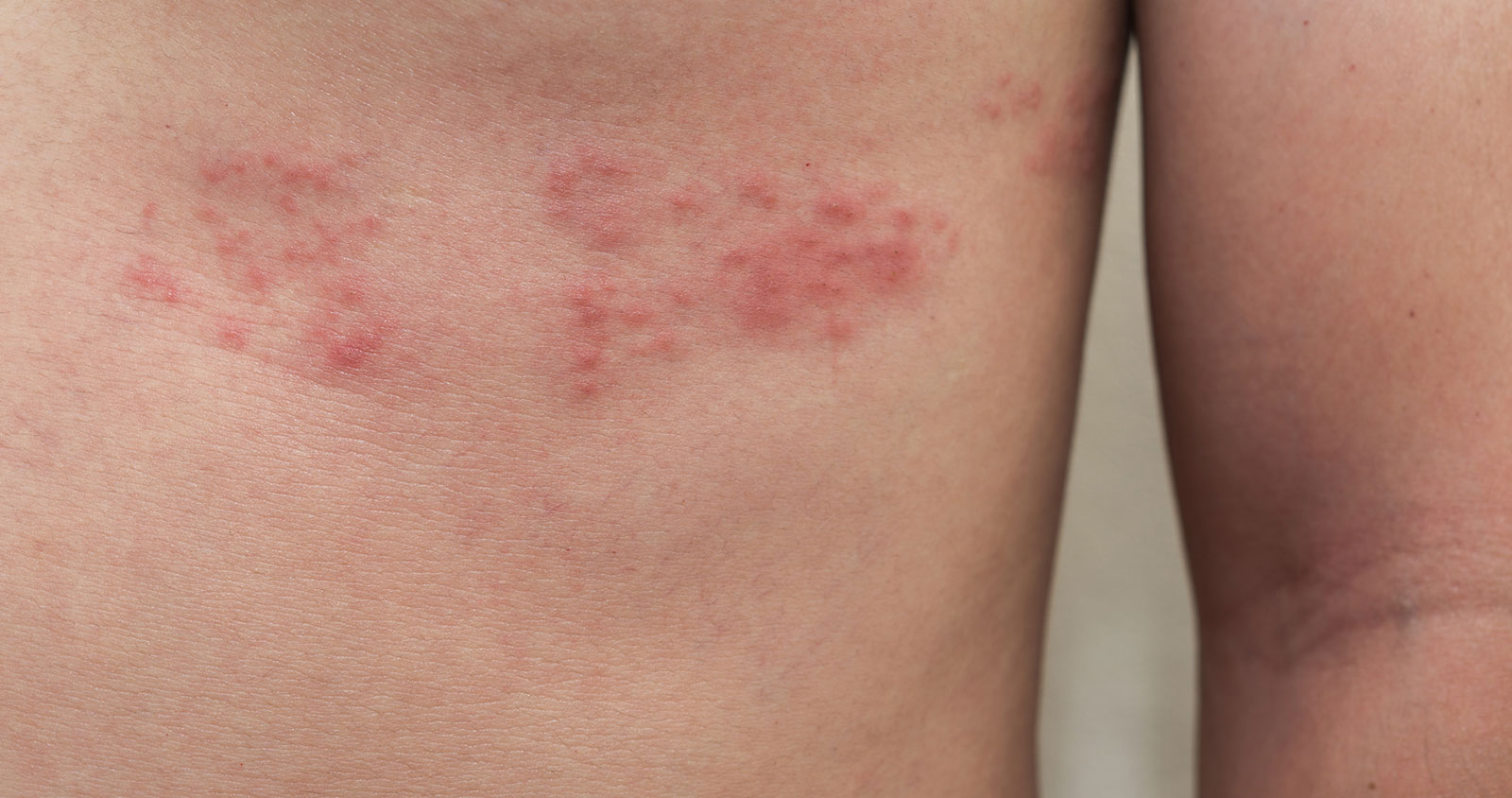
Can kids get shingles after chickenpox?
Yes. Shingles is caused by the same virus that causes chickenpox, called varicella-zoster virus. After a child has chickenpox, the virus does not fully leave the body. It goes quiet and stays in nerve tissue near the spinal cord.
Years later, it can reactivate and travel along a nerve to the skin, causing shingles. That is why shingles tends to show up in a stripe or band on one area of the body.
But my child had the chickenpox vaccine, not chickenpox
Kids who have been vaccinated can still, rarely, get shingles. When it happens after vaccination, it often looks milder. Vaccination also lowers the chance of chickenpox in the first place and appears to lower the overall risk of shingles compared with natural chickenpox infection.
Why would the virus wake up?
Often there is no clear cause. These are better thought of as risk factors, not guarantees:
- Recent illness or fever
- Major stress on the body
- Immune system suppression (for example, certain medications or medical conditions)
- Having had chickenpox very young, including as an infant
If your child has a known immune problem or takes immune-suppressing medication, call your care team promptly if you suspect shingles.
Rash clues parents can use
Shingles can be confusing at first because the earliest symptoms are often not the rash. Many kids feel “off” in a specific spot before anything shows up.
Early symptoms
- Tingling, burning, itching, or tenderness on one area of skin
- Localized pain, even with a normal-looking skin surface
- Low-grade fever or fatigue (sometimes)
What the shingles rash looks like
Most of the time, shingles in kids has a few classic features:
- One side of the body: It usually stays on the left or the right, not both.
- In a line or band: Often wraps around the torso, or follows a stripe on the arm, leg, or face.
- Clusters of blisters: Small fluid-filled bumps on a red base.
- New spots for several days: Then the blisters crust over.
The rash is often on the trunk. It can also appear on the face or near the eye, which needs quick medical attention.
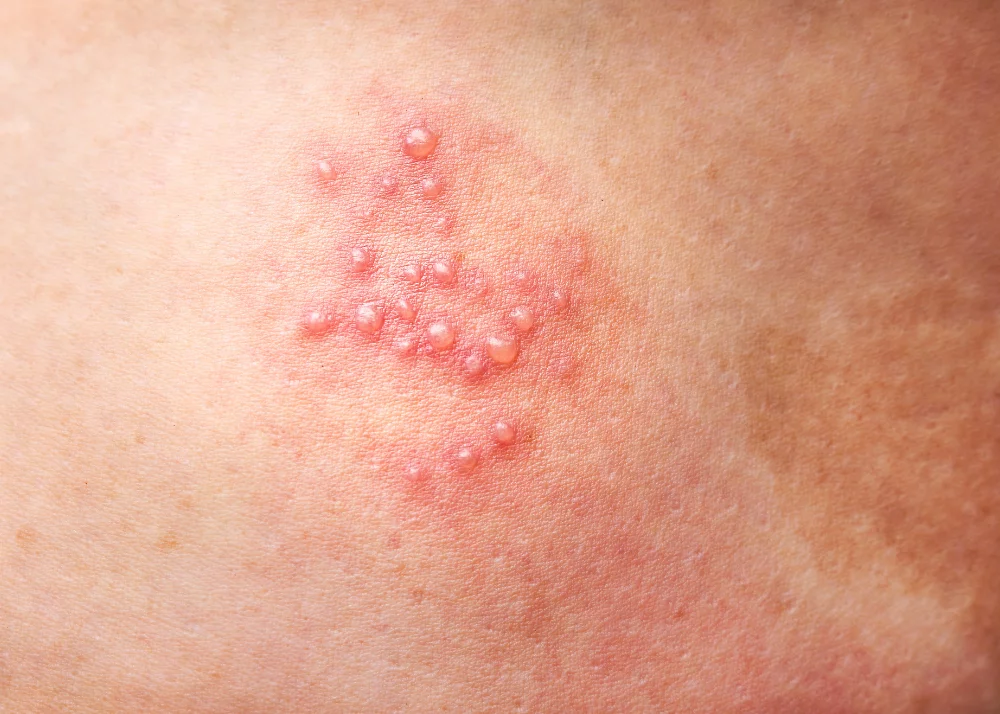
Shingles vs. other common rashes
In real life, shingles is one of those diagnoses that gets mixed up with everyday kid rashes. Here are some practical comparisons.
Shingles vs. chickenpox
- Shingles: Usually one-sided, band-like, clustered blisters in one region.
- Chickenpox: Spots are widespread and scattered over the body, often with lesions in different stages at the same time.
Shingles vs. hand, foot, and mouth
- Hand, foot, and mouth: Mouth sores and rash on hands and feet are common, plus fever.
- Shingles: Follows a nerve path and is typically not focused on hands and feet.
Shingles vs. eczema or contact rash
- Eczema or contact rash: Often symmetrical, scaly, or patchy. It is usually itchy more than painful.
- Shingles: Tends to be tender, burning, or painful with grouped blisters.
If your child is in notable pain, has a one-sided blistering rash, or the rash is near the eye, it is worth a medical call even if you are not 100 percent sure.
Pain and itch care at home
Comfort matters. When kids hurt, sleep disappears, and then everything feels harder. Shingles pain can range from mild to very uncomfortable.
Simple comfort measures
- Cool compresses: A clean, cool, damp cloth on the area for 10 to 15 minutes can reduce itch and sting.
- Loose clothing: Soft cotton reduces rubbing.
- Keep nails short: Scratching can break blisters and raise infection risk.
- Gentle cleansing: Mild soap and water is enough. Pat dry.
Over-the-counter options
For many kids, these are the most helpful and realistic tools:
- Acetaminophen or ibuprofen for pain and fever (use dosing based on your child’s weight and age, and avoid ibuprofen if your clinician has told you not to use it).
- Calamine lotion for itch in some children (avoid eyes and mucous membranes).
- Oral antihistamine for itch at night may help some kids, but ask your pediatrician or pharmacist which one is age-appropriate.
Aspirin note: Do not give aspirin to children because of the risk of Reye syndrome.
When kids need prescription help
Antiviral medication (often acyclovir or similar) may be recommended, especially when started early. Many clinicians aim for treatment within about 72 hours of rash onset, or later in certain cases. If you think your child may have shingles, calling early gives you the most options.

Is shingles contagious?
This part is unintuitive, so take a breath. Shingles is not typically “caught” from someone else the way colds are. A child with shingles generally cannot directly give another person shingles. What they can do is spread varicella-zoster virus to someone who has never had chickenpox and has not been vaccinated. That exposed person could then develop chickenpox.
How it spreads
- The virus spreads mainly through direct contact with fluid from the shingles blisters.
- Airborne spread is uncommon with localized shingles, especially if the rash is covered, but it can be more of a concern with disseminated shingles or in certain healthcare settings.
When it stops being contagious
In general, shingles is considered contagious until all lesions are crusted over and there are no new blisters forming. Once everything is crusted, the risk drops significantly.
School and daycare
Policies vary by location and school, so it is always worth checking your local rules (and the school nurse, if you have one). The medical guidance often depends on whether shingles is localized or widespread.
Localized shingles
Localized means the rash is limited to one area. Many children with localized shingles can attend school or daycare if:
- The rash can be fully covered by clothing or a secure dressing
- Your child feels well enough to participate
- They can follow basic hygiene, like handwashing and not picking at the rash
Even when attendance is allowed, be cautious about contact with high-risk people, including pregnant people who are not immune to chickenpox, newborns, and immunocompromised classmates or teachers. If you are not sure who is high-risk in your setting, ask the school nurse or daycare director.
Disseminated shingles
Disseminated means the rash is widespread, looks more like chickenpox, or appears in multiple areas outside a single band. This is more concerning and can happen in children with weaker immune systems.
Disseminated shingles is treated more like chickenpox from a contagion standpoint. Children generally need to stay home and avoid contact with others until lesions crust over, and they should be evaluated promptly by a clinician.
Diagnosis: what to expect
Many clinicians can diagnose shingles based on the history and the look and location of the rash.
- If the rash is atypical, your clinician may do a swab of a blister for testing (often PCR) to confirm varicella-zoster virus.
- If shingles is near the eye, your child may need urgent evaluation to protect vision.
When to call the doctor
Trust your gut here. Shingles is usually manageable, but there are specific situations where you want medical advice quickly.
Call your pediatrician the same day if:
- The rash is near the eye, on the nose, or on the face
- Your child has moderate to severe pain
- Your child is under 1 year old
- Your child has a weakened immune system or takes immune-suppressing medication
- The rash is widespread or appearing in multiple body areas
- Your child has a high fever, looks very ill, or you are worried about dehydration
Go to urgent care or the ER now if:
- There are signs of eye involvement: eye redness, eye pain, light sensitivity, swelling around the eye, or vision changes
- Your child has severe headache, stiff neck, confusion, or unusual sleepiness
- You see signs of skin infection: rapidly worsening redness, warmth, swelling, pus, or streaking
- Your child has ear pain with a shingles-like rash near the ear, or any facial weakness or drooping
How long shingles lasts in kids
Many children start with tingling or tenderness for a day or two, then the rash appears. New blisters can continue for a few days, then they crust over (often within about 7 to 10 days). For a lot of kids, the whole course is about 2 to 3 weeks, sometimes longer.
One relief for parents: long-lasting nerve pain after shingles (postherpetic neuralgia) is much less common in children than in older adults, but you should still tell your clinician if pain seems out of proportion or continues after the rash heals.
Protecting siblings and relatives
If you have other children at home, especially a baby or an unvaccinated toddler, you are right to think about containment.
- Cover the rash when possible and discourage touching.
- Handwashing is your best friend, especially after applying lotion or changing dressings.
- Do not share towels, washcloths, or bathwater.
- Keep distance from high-risk people until lesions are crusted: pregnant people who are not immune, newborns, and immunocompromised family members.
If you are concerned about a high-risk exposure, call your pediatrician. There are situations where preventive treatment may be recommended for vulnerable contacts, but timing matters.
Prevention and next steps
Routine varicella (chickenpox) vaccination helps prevent chickenpox and also reduces the risk of shingles later compared with having chickenpox infection.
Parents sometimes ask about the shingles vaccine. It is generally recommended for older adults, not children, except in specific high-risk medical situations guided by a specialist.
Quick reassurance
If you are reading this at 3 AM, squinting at a suspicious rash, you are not alone. Shingles can look scary, but in most otherwise healthy kids it is treatable, it is temporary, and it does not mean you missed something as a parent.
When in doubt, take a clear photo in good light, note when symptoms started, and call your pediatrician. That small step often saves a lot of stress and helps get the right care started quickly.