Signs of Food Allergies in Babies
Sarah Mitchell
Sarah Mitchell is a Registered Pediatric Nurse and a mother of three who has spent over a decade helping families navigate the beautiful, chaotic early years of childhood. She combines evidence-based medical knowledge with real-world parenting experience to offer practical, compassionate advice. At Awesome Parent, Sarah's mission is to help exhausted parents find solutions, trust their instincts, and finally get some sleep.
If you are reading this with one hand while the other holds a spoonful of peanut butter toast or scrambled egg, I see you. Starting solids is exciting, messy, and yes, a little nerve-wracking.
Many babies do not have a serious reaction. But reactions can still happen, especially with common allergens, and it helps to know what to look for so you can respond calmly and quickly if something seems off.

This guide covers the most common signs of food allergy in infants and toddlers, what counts as an emergency, how quickly symptoms usually show up, and what to do next.
Quick note: This article is for education, not medical advice. If you are worried about your child, call your pediatrician. If breathing is involved or your child seems very sick, call your local emergency number (911 in the US).
Food allergy vs. food intolerance
Parents often use these terms interchangeably, but they are not the same.
Food allergy
A food allergy involves the immune system. The body treats a food protein like a threat and releases chemicals (like histamine) that can cause symptoms such as:
- Hives or widespread itchy rash
- Swelling of the lips, face, tongue, or eyelids
- Vomiting shortly after eating
- Wheezing or trouble breathing
- Anaphylaxis, a severe, life-threatening reaction
Food allergies can be unpredictable. A mild reaction one day can be more serious another day. That is why we take them seriously.
Food intolerance
Food intolerance usually does not involve the immune system. It is more about digestion. Symptoms are often uncomfortable but not typically life-threatening, such as:
- Gas, bloating
- Loose stools
- Belly pain or fussiness after eating
Important: Some non-IgE food reactions (like certain delayed gut allergies) can look like “intolerance” at first and still need medical care. If your baby repeatedly vomits, has blood in stool, is not gaining weight well, or seems unwell after certain foods, call your pediatrician.
Allergy signs in babies and toddlers
Food allergy symptoms can involve the skin, stomach, breathing, and circulation. You might see one symptom or several at the same time.
Skin symptoms
- Hives: raised, red welts that can move around and come and go
- Flushing: sudden redness of the face or body
- Itching: rubbing face, scratching, or seeming suddenly uncomfortable
- Swelling (angioedema): lips, eyelids, face, tongue, or ears
- Eczema flare: worsening patches after a trigger food (more on this below)
Stomach and gut symptoms
- Vomiting soon after eating (especially repeated or forceful)
- Diarrhea
- Abdominal pain (older toddlers may clutch belly, cry, or curl up)
- Blood or mucus in stool (not typical for an immediate IgE allergy, but always worth calling your pediatrician)
Breathing and airway symptoms
- Coughing that starts right after eating
- Wheezing or noisy breathing
- Hoarse voice or sudden voice change
- Throat tightness (toddlers may say “throat hurts” or refuse to swallow)
- Trouble breathing or working harder to breathe (pulling in at ribs, flaring nostrils)
Whole-body symptoms
- Sudden sleepiness, limpness, or acting “out of it”
- Pale, cool, clammy skin
- Dizziness (in older toddlers)
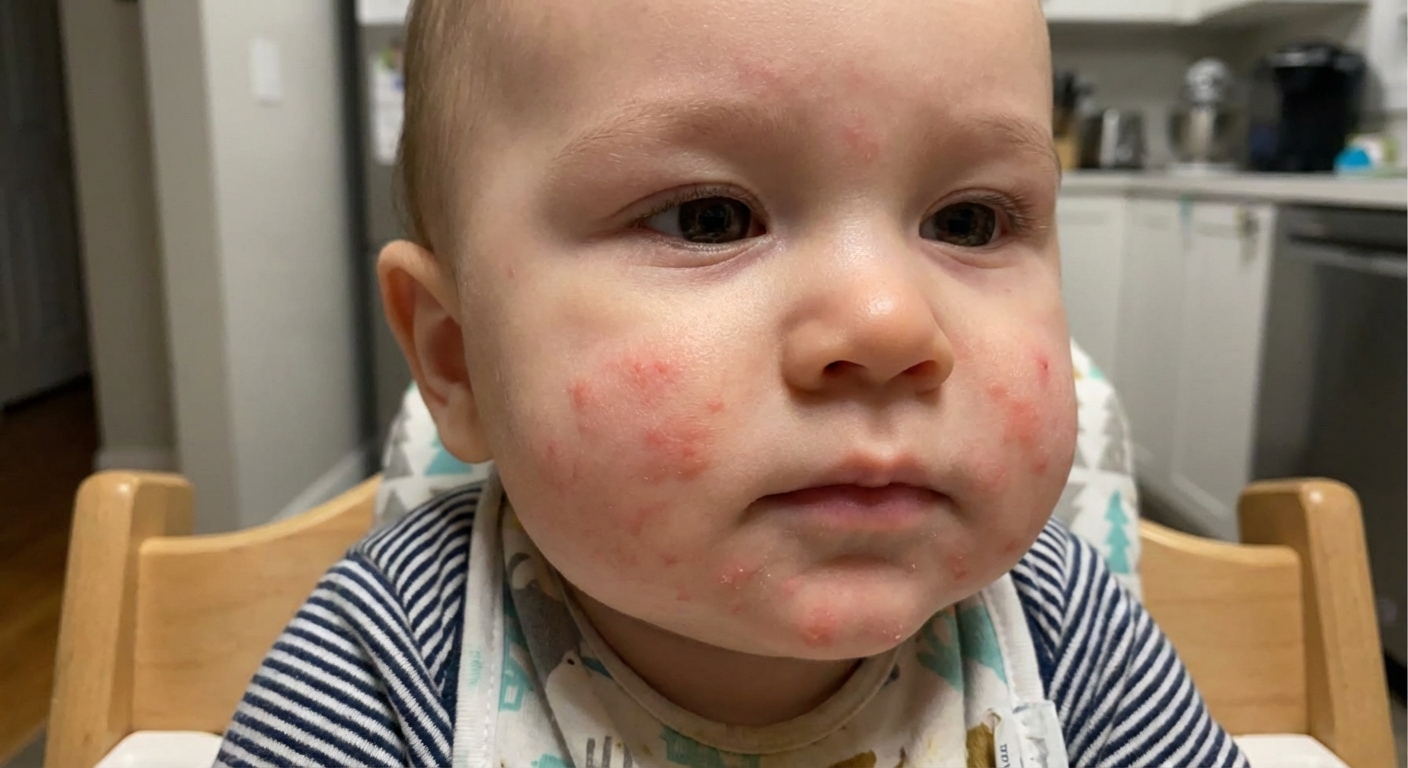
Real-life note: Parents often expect a food allergy to be dramatic. Sometimes it is. Sometimes it is just a couple of hives and a single vomit. Trust your gut. If something feels “different” right after a new food, pause and pay attention.
Choking or allergy?
This is a big one when you are starting solids.
- Gagging is common as babies learn textures. It can look scary, but it is often noisy and the baby is still moving air. It usually improves with experience.
- Choking is an airway emergency. Your baby may be silent or unable to cough or cry, and may turn blue. If you think your baby is choking, follow infant choking first aid and call your local emergency number.
- Allergic reactions tend to cause hives, swelling, vomiting, cough, wheeze, or breathing changes that start after eating. Allergy and choking can happen around the same time, but they are treated differently.
If you are not sure what you are seeing, treat breathing problems as urgent and call for help.
What anaphylaxis can look like
Anaphylaxis is a severe allergic reaction that can affect breathing and blood pressure. It can be life-threatening and needs immediate treatment.
In babies and toddlers, anaphylaxis may look like:
- Difficulty breathing, wheeze, or repetitive coughing
- Swelling of tongue or lips that is getting worse
- Stridor (a high-pitched sound when breathing in)
- Hives plus vomiting or hives plus any breathing trouble
- Repeated vomiting with hives or swelling
- Sudden lethargy, limpness, or collapse
- Pale or bluish color around lips or face
If you suspect anaphylaxis, treat it like an emergency even if you are not 100 percent sure. In pediatrics, we would rather you “overreact” than wait.
How fast do reactions happen?
Timing is one of the biggest clues.
Immediate reactions (classic food allergy)
These are often IgE-mediated reactions. Symptoms typically start:
- Within minutes of eating
- Usually within 2 hours (and occasionally longer)
Hives, swelling, vomiting, coughing, wheezing, and anaphylaxis usually fall into this category.
Delayed reactions
Some food reactions show up later, including certain eczema flares and non-IgE gut reactions. Symptoms may appear:
- Several hours after eating
- Sometimes the next day
One important delayed reaction to know is FPIES (food protein-induced enterocolitis syndrome). It can cause repetitive vomiting, pallor, and sleepiness or limpness, often 1 to 4 hours after a trigger food. It can be serious even without hives or wheeze.
Call your pediatrician right away for suspected FPIES. If your baby is very sleepy or limp, looks pale, cannot keep fluids down, or seems dehydrated, seek emergency care.
If delayed symptoms are consistent with a specific food, talk with your pediatrician or an allergist before removing lots of foods from your baby’s diet.
Top food allergens for little kids
Any food can cause an allergy, but a handful cause the majority of reactions in early childhood:
- Cow’s milk
- Egg
- Peanut
- Tree nuts (like cashew, walnut, almond)
- Sesame
- Soy
- Wheat
Other common allergens include fish and shellfish, depending on where you live and what foods your family eats.
Eczema and food allergies
If your baby has eczema, you have probably wondered if food is to blame. Here is the calm truth: eczema and food allergies are linked, but one does not automatically mean the other.
- Babies with moderate to severe eczema have a higher risk of food allergy.
- But most eczema flares are triggered by things like dry skin, saliva, heat, soaps, illness, or environmental allergens.
A food allergy is more likely when an eczema flare happens along with other symptoms, especially hives, swelling, vomiting, or respiratory symptoms soon after eating.
If you suspect a pattern, keep notes and bring them to your child’s clinician. Please avoid doing broad food elimination on your own, because babies need variety for nutrition and continued exposure can help maintain tolerance for some foods.
What to do if your baby reacts
When your baby reacts, your job is not to be perfect. Your job is to be safe.
Step 1: Stop the food and check
- Take the food away and wipe hands and face.
- Look for hives, swelling, and any breathing changes.
- Notice behavior: unusually sleepy, floppy, or extremely fussy.
Step 2: Decide if it is an emergency
Call 911 right away (or your local emergency number) if your baby has any of the following:
- Trouble breathing, wheezing, repetitive coughing
- Swelling of the tongue or throat, drooling or trouble swallowing
- Blue or gray lips, or looks pale and very ill
- Fainting, limpness, or sudden extreme sleepiness
- Widespread hives plus vomiting or any breathing symptoms
Call your pediatrician urgently (same day) if:
- There are hives or swelling but your child is breathing comfortably and acting mostly normal
- There is vomiting shortly after a new food, even without hives
- There is vomiting that starts hours later and repeats (possible FPIES), even if there is no rash
- There is persistent diarrhea after a suspected trigger food
Monitor at home if symptoms are mild and resolve quickly, but still report it to your pediatrician:
- A few small hives around the mouth that go away
- Mild redness without other symptoms
Step 3: Position your child safely
- If your child seems faint, floppy, very pale, or seriously unwell, lay them flat on their back if possible.
- If vomiting is happening or your baby is uncomfortable flat, place them on their side to protect the airway.
- If breathing is clearly difficult, it is okay to let them sit in a position that makes breathing easiest.
- Avoid suddenly standing them up or holding them upright if they seem faint. During anaphylaxis, abrupt upright posture can worsen low blood pressure.
Step 4: Use epinephrine if prescribed
If your child has an epinephrine auto-injector and you suspect anaphylaxis, use epinephrine right away. Do not wait to see if it gets worse. Epinephrine is the first-line treatment for anaphylaxis.
How to use it in babies and toddlers (general guidance):
- Inject into the outer mid-thigh. It can go through clothing.
- Hold your child’s leg still during injection.
- Follow the instructions for your specific device, since timing and steps can vary.
- After giving epinephrine, call 911 or have someone call for you.
Device reminder: Epinephrine auto-injectors come in different doses. Ask your clinician which device is right for your child’s weight.
When in doubt: If you are deciding between epinephrine and not, and symptoms suggest anaphylaxis, choose epinephrine. Delaying epinephrine is associated with worse outcomes.

Step 5: Get emergency help for severe symptoms
If there are breathing symptoms, severe swelling, limpness, or your baby seems very ill, call an ambulance. Emergency teams can support breathing and give additional medications en route.
Step 6: Document and follow up
Write down:
- The exact food and how it was prepared
- How much was eaten
- When symptoms started
- What symptoms occurred
- What you gave (epinephrine, antihistamine) and when
Then schedule follow-up with your pediatrician and, often, a pediatric allergist.
Where antihistamines fit
Antihistamines can help with itching and hives, but they do not treat anaphylaxis. They do not open the airway or prevent shock.
If your child has only mild hives and is otherwise well, your clinician may recommend an age-appropriate antihistamine dose. If there are any breathing symptoms, significant swelling, or whole-body symptoms, epinephrine comes first and you call 911.
Because dosing depends on age and weight, use antihistamines for infants only with your pediatrician’s guidance.
What not to do
- Do not “wait it out” if there are breathing symptoms, swelling of the mouth or tongue, or repeated vomiting with hives.
- Do not rely on a bath, oils, or home remedies to stop hives.
- Do not give food or drink if your baby is having trouble swallowing or seems very sleepy or floppy.
- Do not re-try the suspected food at home until you have medical guidance.
After a reaction: next steps
1) Get an evaluation
If your baby had hives, swelling, vomiting soon after eating a particular food, repeated delayed vomiting, or any severe reaction, ask your pediatrician about referral to a pediatric allergist. Testing may include skin testing or blood testing, plus a careful history. Sometimes a supervised oral food challenge is recommended.
2) Make a plan for caregivers
If an allergy is diagnosed (or strongly suspected), ask for a written action plan. Make sure anyone feeding your child knows:
- What foods to avoid
- Early symptoms
- When to use epinephrine
- When to call emergency services
3) Keep offering tolerated foods
It is understandable to want to pause solids entirely after a scare. But in many cases, your pediatrician will want your baby to keep eating a variety of foods they have already tolerated.
And once an allergenic food (like peanut or egg) is introduced and tolerated, many clinicians recommend continuing to include it regularly in an age-appropriate form. This helps support ongoing tolerance. Ask your pediatrician or allergist what schedule makes sense for your child.
Call 911 vs. call the pediatrician
If you want the simplest version, here it is.
Call 911 now
- Any trouble breathing, wheezing, repetitive cough
- Swelling of tongue or throat, drooling, trouble swallowing
- Blue or gray color, pale and floppy, fainting
- Hives plus vomiting or any breathing symptoms
- You gave epinephrine (you still need emergency evaluation)
Call your pediatrician soon
- Hives without breathing symptoms
- Swelling limited to lips or around eyes but breathing is normal
- Vomiting shortly after a specific food, especially if it happens more than once
- Repetitive vomiting that starts 1 to 4 hours after a food (possible FPIES), even without hives
- Consistent delayed GI symptoms or eczema flares linked to a food
The 3 AM nurse version: If your baby’s breathing changes or they seem suddenly “not right,” you do not need permission to call 911.
Quick checklist for new foods
- Introduce new foods when your baby is healthy, not during a fever or stomach bug.
- Try new allergenic foods earlier in the day so you can observe for a couple of hours.
- Start with a small amount, then gradually increase if tolerated.
- Know your local emergency number and have a charged phone nearby.

If your baby has severe eczema, a known food allergy, or a strong family history of allergies, ask your pediatrician about the safest way to introduce allergenic foods. Some families benefit from guidance before the first taste.
FAQ
Can a baby react the first time?
Yes. A reaction can happen on the first known exposure. Sensitization can occur through tiny exposures in the environment or through skin contact, especially in babies with eczema.
Do reactions always get worse?
Not always, but they can. Because severity is hard to predict, any suspected allergy deserves medical follow-up.
Is a rash around the mouth always an allergy?
Not necessarily. Some foods (like tomatoes or citrus) can irritate the skin. But if you see hives, swelling, vomiting, cough, wheeze, or the rash spreads, treat it as a possible allergy and contact your pediatrician.
A final word from a nurse mom
Watching your baby react to a food is scary, even if the symptoms are mild. You are not overreacting. You are learning your child, and that is what good parenting looks like.
If you are ever unsure, call your pediatrician. And if breathing is involved or your baby seems very sick, call your local emergency number. You do not have to figure this out alone.