Spider Bites on Kids and Teens: What’s Normal vs When to Worry
Sarah Mitchell
Sarah Mitchell is a Registered Pediatric Nurse and a mother of three who has spent over a decade helping families navigate the beautiful, chaotic early years of childhood. She combines evidence-based medical knowledge with real-world parenting experience to offer practical, compassionate advice. At Awesome Parent, Sarah's mission is to help exhausted parents find solutions, trust their instincts, and finally get some sleep.
As a pediatric nurse and a mom who has done plenty of middle-of-the-night “What is that?” skin checks, I can tell you this: most marks that families call a spider bite are not dangerous. Many are actually mosquito bites, minor allergic reactions, or small skin infections that just happened to show up overnight.
The goal is not to identify the exact spider species. The goal is to keep your child comfortable, prevent infection, and recognize the small number of situations that truly need same-day medical care.
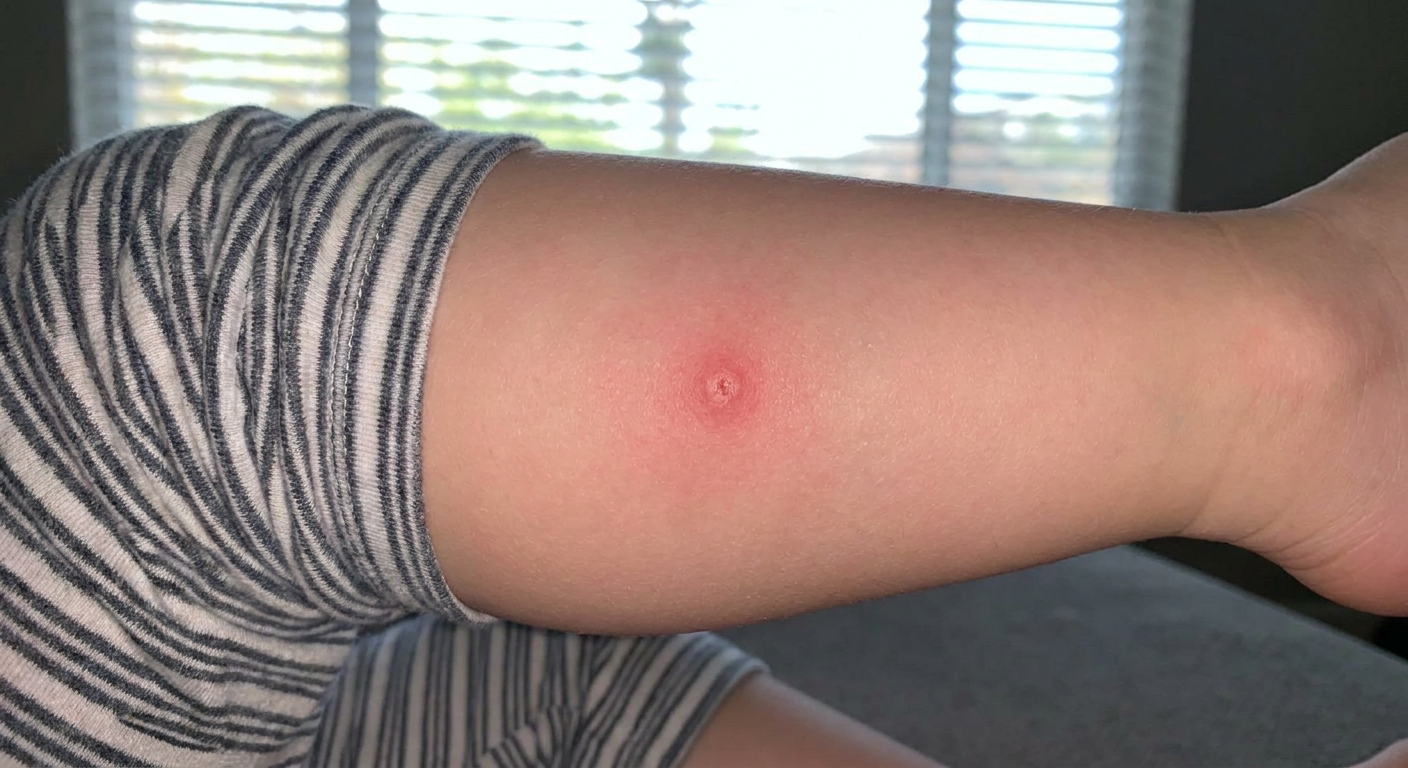
First: What a mild bite can look like
A typical mild bite or sting tends to stay localized and slowly improves over a few days.
- A small red bump, sometimes with a tiny dot in the center
- Itching that is more annoying than painful
- Mild swelling around the spot
- Redness that peaks early and does not keep spreading quickly (a little change in the first 24 to 48 hours can be normal)
- No fever and your child otherwise acts like themselves
If it looks like this, home care and close watching is usually enough.
Why “spider bite” is often a mislabel
In clinic, we see a lot of “spider bites” that are actually:
- Mosquito, flea, or bed bug bites (often multiple, often itchy)
- Hives or contact irritation from plants, soaps, or sports gear
- Ingrown hairs or irritated follicles, especially in teens
- Early skin infections like a small boil or abscess (including staph, sometimes MRSA)
This is one reason I encourage parents to focus less on the creature and more on the pattern: is it staying mild, or is it escalating?
What to do at home
Step 1: Clean it
Wash the area with soap and running water. If the skin is broken or your child scratched it raw, a thin layer of plain petroleum jelly can help protect it while it heals. Cover with a small bandage if it is in a spot that gets rubbed by socks, waistbands, or sports gear.
Step 2: Calm itch and swelling
- Cool compress for 10 minutes at a time, a few times a day
- Elevate the arm or leg when you can, especially if swelling is noticeable
- Oral antihistamine (like cetirizine or loratadine) can help itching in many kids and teens. Follow the package dosing or your clinician’s advice.
- 1% hydrocortisone can help itching on unbroken skin, used sparingly. Avoid on open sores, near the eyes, and on genitals. If your child is very young, or if you think the area may be infected, check with a clinician first.
- Discourage scratching by trimming nails and using a bandage if needed
Step 2.5: Help with pain if needed
If it is sore (not just itchy), you can consider acetaminophen or ibuprofen as directed on the label and your pediatrician’s guidance.
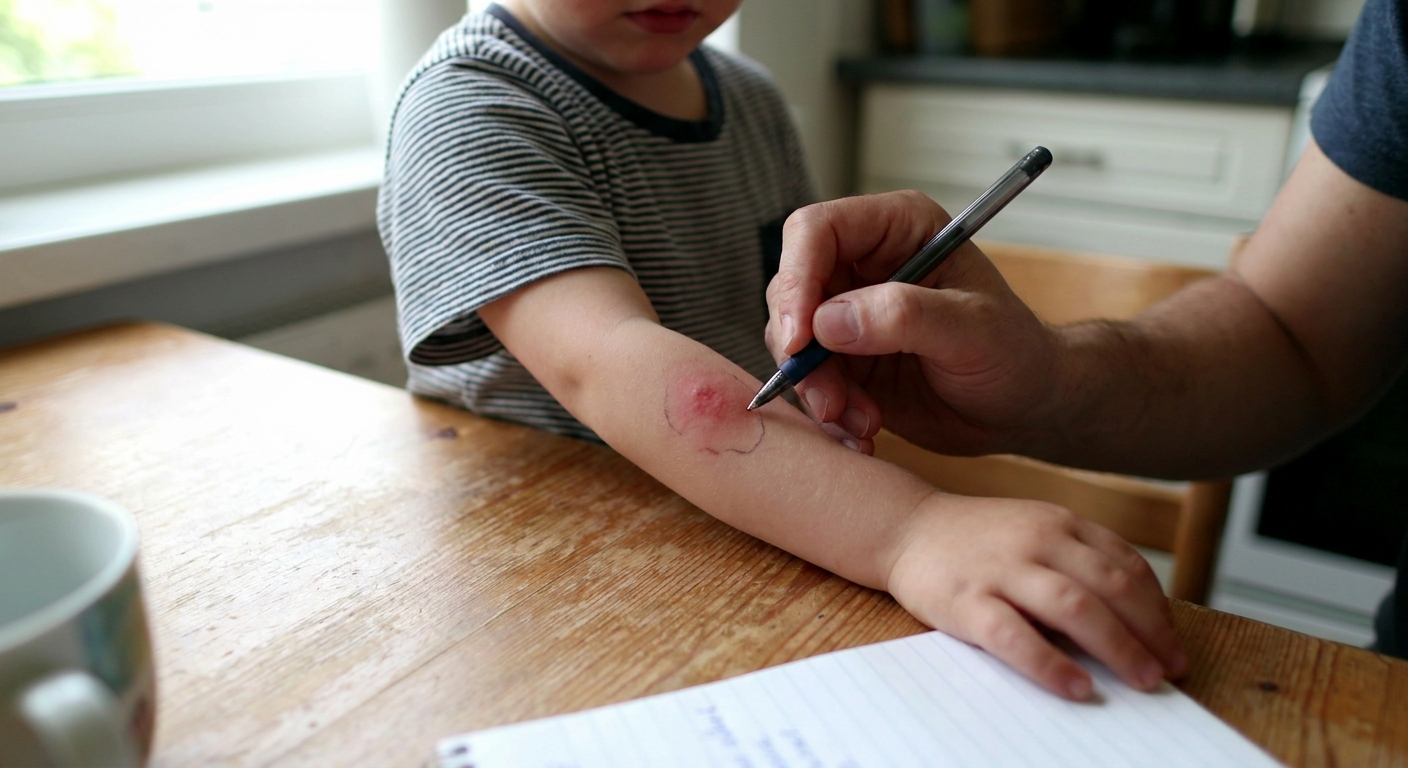
Step 3: Mark and measure
If the area is red, use a pen to lightly trace the edge of the redness on the skin and write the time. This simple trick makes it much easier to tell if it is spreading.
Step 4: Take a daily photo
A clear photo in good light once a day can help you notice subtle changes and can be very helpful if you end up calling the nurse line.
Call a clinician: signs it is not staying mild
Reach out to your child’s pediatrician, urgent care, or nurse line if you notice:
- Redness that keeps expanding or is spreading quickly over hours
- Increasing warmth around the spot
- Worsening pain (itching is common, escalating pain is more concerning)
- Swelling that is significant or limiting movement of a finger, toe, wrist, or ankle
- Pus, crusting, or a draining blister
- A firm, tender lump that looks like a boil forming
- Red streaking traveling away from the area
- Fever or your child seems unusually tired or unwell
- It is on the face, around the eye, genitals, or hands where swelling can cause bigger problems
These can be signs of a skin infection or a stronger inflammatory reaction, and a clinician may want to examine it.
Extra note: If your child is an infant, immunocompromised, or has significant eczema or skin breakdown, use a lower threshold to call.
Go now: urgent and emergency red flags
Some symptoms are “call today,” and some are “go now.” When in doubt, call your local nurse line or seek urgent evaluation.
Call 911 or go to the ER now
- Trouble breathing, wheezing, repetitive coughing, or throat tightness
- Swelling of lips, tongue, or face
- Fainting, extreme dizziness, confusion
- Widespread hives plus other symptoms (vomiting, breathing trouble, lethargy)
If your child has a known anaphylaxis plan and an epinephrine auto-injector, follow that plan first and then seek emergency care.
Same-day urgent evaluation
- Severe, rapidly worsening pain that seems out of proportion to the skin finding
- Repeated vomiting, severe headache, or neck stiffness
- High fever with a rapidly worsening skin lesion
- Any fever in a baby under 3 months should prompt immediate medical advice
- Dusky, gray, or rapidly spreading discoloration around the wound
Antibiotics: when they help and when they do not
This part surprises many families: clinicians do not give antibiotics just because something is called a “spider bite.” Antibiotics are used when there are signs of a bacterial skin infection, such as cellulitis or an abscess.
Antibiotics may be considered when there is:
- Expanding redness with warmth and tenderness
- Fever or your child looks ill
- Drainage, pus, or a boil (sometimes a culture is taken)
- It is worsening, or not improving as expected, especially with warmth, tenderness, and spreading
What else a clinician might do
- Drain an abscess if one forms (this is often the key step). Antibiotics are not always needed for a simple, well-drained abscess without surrounding cellulitis, but that is a clinician call.
- Recommend pain control and warm compresses if a boil is developing
- Review tetanus status if there is an open wound. A booster may be recommended depending on the wound and when the last dose was given.
Important: do not use leftover antibiotics or someone else’s prescription. Wrong medication or dosing can make things worse and can delay the right care.
Geography without panic
Some regions have spiders that can cause more significant reactions, but most bites in most places are still mild. The two names parents most often worry about are the Black Widow and the Brown Recluse.
- Focus on symptoms, not online photo matching
- Seek care if your child has systemic symptoms (fever, vomiting, muscle cramping, severe pain) or a rapidly worsening wound
- If you happen to safely capture the spider (no bare hands), a photo may help clinicians, but it is not required
Try not to let fear-mongering headlines convince you that every bump is dangerous. Your child’s overall condition and the lesion’s behavior over time matter most.

Blisters, bruising, and rings
Blistering
A small blister can happen from irritation or a stronger local reaction. Keep it clean, avoid popping it, and cover it if it will rub. Call your clinician if blistering is spreading, very painful, or accompanied by fever.
Bruise-like color
Skin can look purple or bruised from inflammation or from scratching. If discoloration is expanding, the area is very painful, or the skin looks dusky or gray, get same-day medical evaluation.
Ring-shaped redness
Some bites and skin irritations can look ring-shaped. A steadily enlarging ring, especially after outdoor exposure in tick-prone areas, is worth a call to your pediatrician because it can be seen with Lyme disease. A helpful rule of thumb is that the classic Lyme rash (erythema migrans) typically expands over days and is often larger than 5 cm, but it is not always a perfect bullseye. Not every ring is Lyme, and not every Lyme rash looks like a ring, so it is best handled with a quick clinical review.
Prevent future bites
- Shake out shoes, sports gear, and stored blankets if they have been sitting in a garage, shed, or basement
- Use gloves for moving firewood, yard cleanup, and cleaning storage areas
- Reduce clutter near beds and in closets where critters can hide
- Keep screens and door sweeps in good shape
- Use age-appropriate insect repellent for outdoor play when bugs are heavy, and follow label directions
If your child keeps getting multiple itchy bites, especially after sleep, consider checking bedding and pets for fleas or bed bugs and loop in your pediatrician if you are not sure what you are dealing with.
And yes, I am also a fan of the simple bedtime check when kids have been playing in dusty corners or helping in the garage. Not because spiders are everywhere, but because tiny problems are easier to handle early.
Quick checklist
If you want a simple gut-check, here it is.
Usually OK to watch
- Small itchy bump
- Mild redness that is not rapidly expanding
- No fever
- Your child is acting normally
Call a clinician
- Redness is spreading quickly, the skin feels hot, or it is getting more tender
- Increasing pain
- Pus, draining, or a boil is forming
- Fever or your child seems unwell
- On face or near the eye
Urgent or emergency care
- Breathing trouble, facial swelling, fainting
- Severe symptoms like repeated vomiting, intense muscle cramps, confusion
- Rapidly worsening wound with significant pain or dusky discoloration
If you are on the fence, trust the part of you that says, “This feels different.” You are not overreacting by calling. You are parenting.
One last nurse-mom note
You do not need to solve the mystery of what bit your kid to take great care of it. Clean it, calm the itch, track the redness, and watch your child’s overall behavior. If the skin is spreading quickly, warming, getting more painful, or your child is sick, that is your cue to bring in backup.
And if you are reading this at 3 AM with your phone flashlight, I am sending you a very sincere “you’re doing great” from my side of the internet.