Strawberry Birthmarks (Infantile Hemangiomas)
Sarah Mitchell
Sarah Mitchell is a Registered Pediatric Nurse and a mother of three who has spent over a decade helping families navigate the beautiful, chaotic early years of childhood. She combines evidence-based medical knowledge with real-world parenting experience to offer practical, compassionate advice. At Awesome Parent, Sarah's mission is to help exhausted parents find solutions, trust their instincts, and finally get some sleep.
If you have noticed a bright red spot on your baby that seems to be getting bigger, you are not alone. Infantile hemangiomas are very common in babies. They are often casually called “strawberry birthmarks,” especially when they are superficial, bright red, but not every “strawberry mark” is a hemangioma.
Here is the reassuring part: many infantile hemangiomas are harmless and improve over time without treatment. Some do leave behind mild skin changes, and a smaller group need treatment to prevent complications. The key is knowing what is expected growth, what needs monitoring, and when to get help sooner.
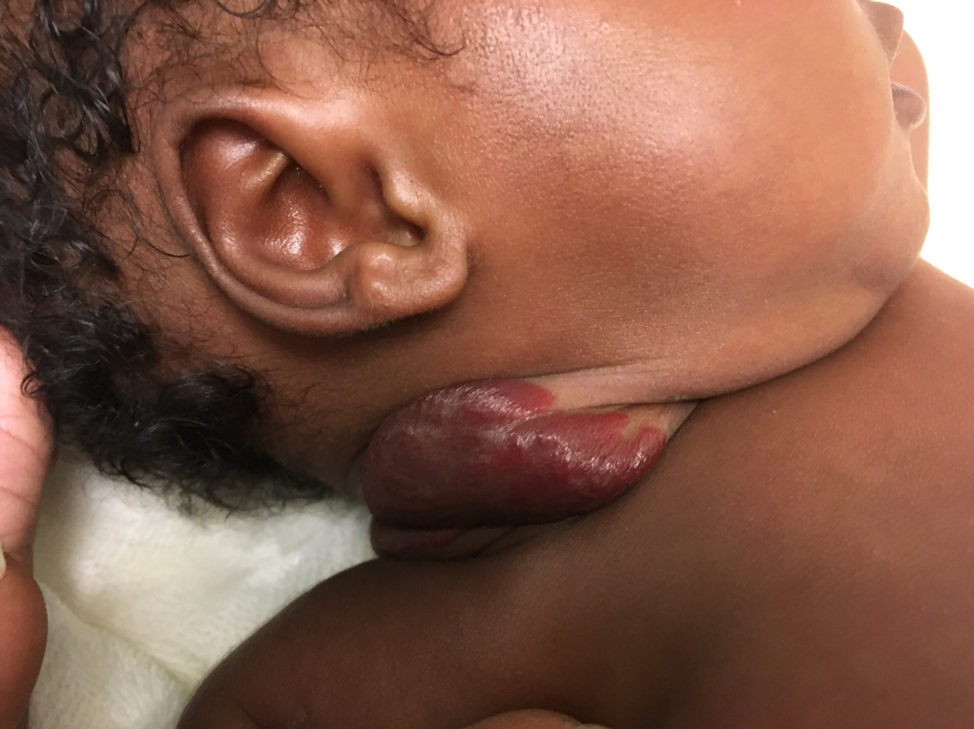
What is an infantile hemangioma?
An infantile hemangioma is a benign (non-cancerous) growth of blood vessels in the skin. They often show up in the first weeks of life. Some are flat and red at first, then become raised. Others sit deeper under the skin and look more bluish or like a soft lump.
Common locations
- Head and neck (very common)
- Trunk
- Arms and legs
- Diaper area (more prone to irritation and ulceration)
Hemangiomas are not caused by anything you did during pregnancy or after birth. They are just one of those newborn surprises no one warns you about.
Quick timeline
- Weeks 1 to 4: often first noticed
- Months 1 to 5: usually the fastest growth period
- Months 6 to 9: some continue meaningful growth, especially deeper lesions
- After infancy: gradual fading and flattening over years
Two stages: growth then fading
Hemangiomas typically follow a predictable pattern with two major phases.
1) Proliferative phase (growth)
This is the “getting bigger” stage. It usually starts in the first weeks of life and is fastest during early infancy. Many hemangiomas grow most rapidly between about 1 to 3 months of age. Growth often slows by around 5 months, though some (especially deeper ones) can keep growing noticeably out to 6 to 9 months.
During this phase you might notice:
- More intense red color
- It becoming raised or thicker
- Edges expanding outward
- For deeper hemangiomas, a fuller, bluish swelling under the skin
2) Involution phase (fading and shrinking)
After growth slows, hemangiomas gradually begin to flatten and lighten. This happens over years, not weeks. Many improve a lot by preschool age. Some leave behind mild skin changes like extra skin, a faint stain, or tiny visible blood vessels.
If you are watching one and thinking, “It looks worse before it looks better,” that is often true, especially in the first few months.
How to monitor at home
In triage, I used to tell parents: we are not trying to win a photography award. We just want a simple, consistent record so we can tell whether it is following the expected pattern.
Simple monitoring tips
- Take one photo per week in the same lighting and angle.
- Include a size reference like a coin or your clean fingertip nearby (not touching an irritated spot).
- Note the date and any changes: thicker, brighter, scabbing, bleeding, baby seems bothered.
- Watch function: is it near the eye, nose, mouth, or diaper area where it could interfere with vision, breathing, feeding, or get rubbed raw?
If your baby has a routine well visit coming up, bring the photos. They can be incredibly helpful for your pediatrician.

When it is more than cosmetic
Most hemangiomas are low-risk. A smaller group are considered higher-risk because of location, size, depth, or because they are causing skin breakdown or interfering with normal function.
Call your pediatrician promptly if you notice
- Near the eye or eyelid: anything that could block vision or change the eyelid shape needs early assessment.
- On or near the nose or lips: can affect feeding, breathing through the nose, or later shape.
- In the beard area (chin, jawline, neck): this distribution can be associated with airway hemangiomas in some infants.
- Inside the mouth or on the tongue
- In the diaper area: higher friction and moisture increases risk of painful ulceration.
- Rapid change, like dramatic growth over days, sudden swelling, or expansion that seems to double quickly.
- Ulceration (an open sore), crusting with pain, or signs of infection like spreading redness, warmth, swelling, or pus
- Bleeding that does not stop with gentle pressure
- Multiple hemangiomas, especially 5 or more: your clinician may consider whether any additional evaluation is needed (for example, to look for hemangiomas in the liver).
Seek urgent care now if
- Your baby has noisy breathing (stridor), breathing difficulty, or signs of respiratory distress
- A hemangioma near the eye is associated with sudden eyelid drooping or the eye seems blocked
- Bleeding is heavy or will not stop after 10 minutes of steady, gentle pressure
Most parents worry about “cancer.” Hemangiomas are benign. The urgent concerns are typically about function (vision, breathing, feeding) and skin complications like ulceration.
Could it be something else?
Not every red or purple mark is a hemangioma. Your pediatrician may consider other possibilities, especially if the spot was fully formed at birth or is not following the typical growth pattern.
- Capillary malformation (port-wine stain): usually present at birth and tends to grow with the child rather than shrink.
- Bruising or a healing mark from birth trauma
- Vascular malformation: often present from birth and does not have the same “grow then fade” pattern.
- Pyogenic granuloma: a small, fast-growing, very bleed-prone bump (more common in older infants and children).
- Rash, petechiae, or infection: if your baby seems unwell or the skin changes look widespread, get prompt medical advice.
Primary care vs dermatology
Your pediatrician or family doctor is often the right first stop. Many hemangiomas can be safely monitored in primary care, especially if they are small, not in a high-risk location, and not ulcerating.
When primary care monitoring is often enough
- Small hemangioma on the trunk or limb
- Not rapidly enlarging
- No ulceration or bleeding problems
- Not near eyes, airway, mouth, or diaper area
When an early dermatology referral is wise
- High-risk location (eye, nose, lips, beard area, diaper area)
- Large or “segmental” pattern (spreads like a broader patch or band, not a small round bump)
- Rapid growth in early weeks
- Ulceration or significant pain
- Concern for scarring or distortion of normal anatomy
- Parents are feeling stuck or worried and need a clear plan
If treatment might be needed, earlier evaluation is helpful because the best window to slow growth is usually during the proliferative phase.
Large segmental hemangiomas and screening
Some larger hemangiomas, especially those with a segmental pattern in certain locations, can be associated with other findings. This is not something you need to diagnose at home, but it is a good reason for early referral.
- Large segmental hemangiomas on the face or scalp: your clinician may consider evaluation for PHACE association.
- Hemangiomas in the lower back, buttocks, groin, or perineal area: your clinician may consider evaluation for associations sometimes grouped under names like LUMBAR/PELVIS/SACRAL.
If screening is needed, your pediatrician or specialist will explain what they are looking for and why.
Treatment options
Not every hemangioma needs treatment. When we do treat, the goal is usually to prevent complications (like vision problems or ulceration) or to reduce the chance of lasting skin changes in a high-impact area.
1) Watchful waiting
This is the most common plan. It means regular check-ins and photos, with a low threshold to re-evaluate if the spot starts changing quickly or causing problems.
2) Propranolol
Propranolol is a beta-blocker medicine that has become a first-line treatment for many problematic infantile hemangiomas. It can help slow growth and encourage shrinking, especially when started early in the growth phase.
What parents should know:
- It is prescribed and monitored by clinicians experienced with infant hemangiomas.
- Your baby may need a baseline exam and, in some cases, additional monitoring depending on age and health history.
- Families get specific safety instructions, especially around feeding routines, because beta-blockers can affect blood sugar if a baby is not eating well.
- Other possible side effects your clinician may review include sleep changes, cool hands and feet, and wheezing in susceptible infants.
If your clinician recommends propranolol, ask: “What signs should make me pause a dose and call you?” A good plan should feel clear and doable.
3) Topical beta-blocker
For some small, thin, superficial hemangiomas, a topical beta-blocker may be considered. This is not right for every case, but it can be an option your pediatrician or dermatologist discusses depending on size and location.
4) Laser
Laser may be used in certain situations, such as:
- Helping an ulcerated hemangioma heal
- Treating residual redness or small visible vessels after involution
- Select superficial lesions when medication is not appropriate
Laser decisions are individualized, and they are typically managed by pediatric dermatology or a specialized vascular anomalies team.
5) Surgery
Surgery is not a typical early treatment for most hemangiomas. It may be considered later for selected cases when there is leftover stretched skin or contour changes after the hemangioma has shrunk.

Ulceration
If there is one complication I want parents to recognize early, it is ulceration. This is when the skin over the hemangioma breaks down into a sore. It can be very painful and can get infected.
Signs of ulceration
- A white or gray area developing on the hemangioma
- Cracking, scabbing, or an open sore
- Baby seems very uncomfortable when the area is touched or during diaper changes
- Bleeding with minimal friction
Ulceration is treatable, but it should be evaluated promptly. Do not wait for the next routine checkup if you suspect it.
Airway hemangiomas
Airway hemangiomas are uncommon, but they matter because they can affect breathing. One clue clinicians pay attention to is a hemangioma pattern in the “beard area,” which can include the chin, jawline, and front of the neck. When airway hemangiomas happen, symptoms often show up in early infancy and can worsen as hemangiomas grow.
Call your clinician urgently if your baby has:
- Noisy breathing that is new or worsening
- High-pitched sound when breathing in
- Retractions (skin pulling in at the ribs or neck with breaths)
- Color changes (blue or gray around lips)
To be clear, a hemangioma on the neck does not automatically mean an airway problem. We use the full clinical picture, and when needed, specialists can evaluate safely.
Questions to ask
- Does this look like an infantile hemangioma, or could it be something else?
- Is it in a high-risk location or likely to ulcerate?
- How often should we check in, and what changes should prompt a sooner call?
- Do you recommend dermatology or a vascular anomalies clinic referral now?
- If treatment is recommended, what is the goal: function, comfort, preventing scarring, or cosmetic improvement?
The bottom line
Infantile hemangiomas can be startling, especially during the early growth phase. Most are harmless and improve with time. The ones we take more seriously are the ones that affect vision, breathing, feeding, or skin integrity, or that are in high-risk areas like the eye, lips, diaper region, or beard distribution.
If you are unsure, take a few clear photos and message or call your pediatrician. You do not have to figure this out alone at 3 AM. That is what we are here for.
Quick reassurance: “Getting bigger” is often expected early on. “Getting in the way” of normal breathing, seeing, feeding, or “breaking down into a sore” is what deserves faster attention.