Stye in Kids: Causes, Treatment, and How Long It Lasts
Sarah Mitchell
Sarah Mitchell is a Registered Pediatric Nurse and a mother of three who has spent over a decade helping families navigate the beautiful, chaotic early years of childhood. She combines evidence-based medical knowledge with real-world parenting experience to offer practical, compassionate advice. At Awesome Parent, Sarah's mission is to help exhausted parents find solutions, trust their instincts, and finally get some sleep.
If your child wakes up with a tender, red bump on their eyelid, it is easy to assume it is pink eye, a bug bite, or something mysterious they picked up at preschool (because of course). The good news is that a stye is usually a minor infection that improves with simple home care.
As a pediatric nurse and a mom, I will tell you the most helpful thing right up front: most styes are not an emergency, and squeezing them is the fastest way to make a small problem into a bigger one. Let’s walk through what is going on, what you can do tonight, and when it is time to call your child’s clinician.
What is a stye?
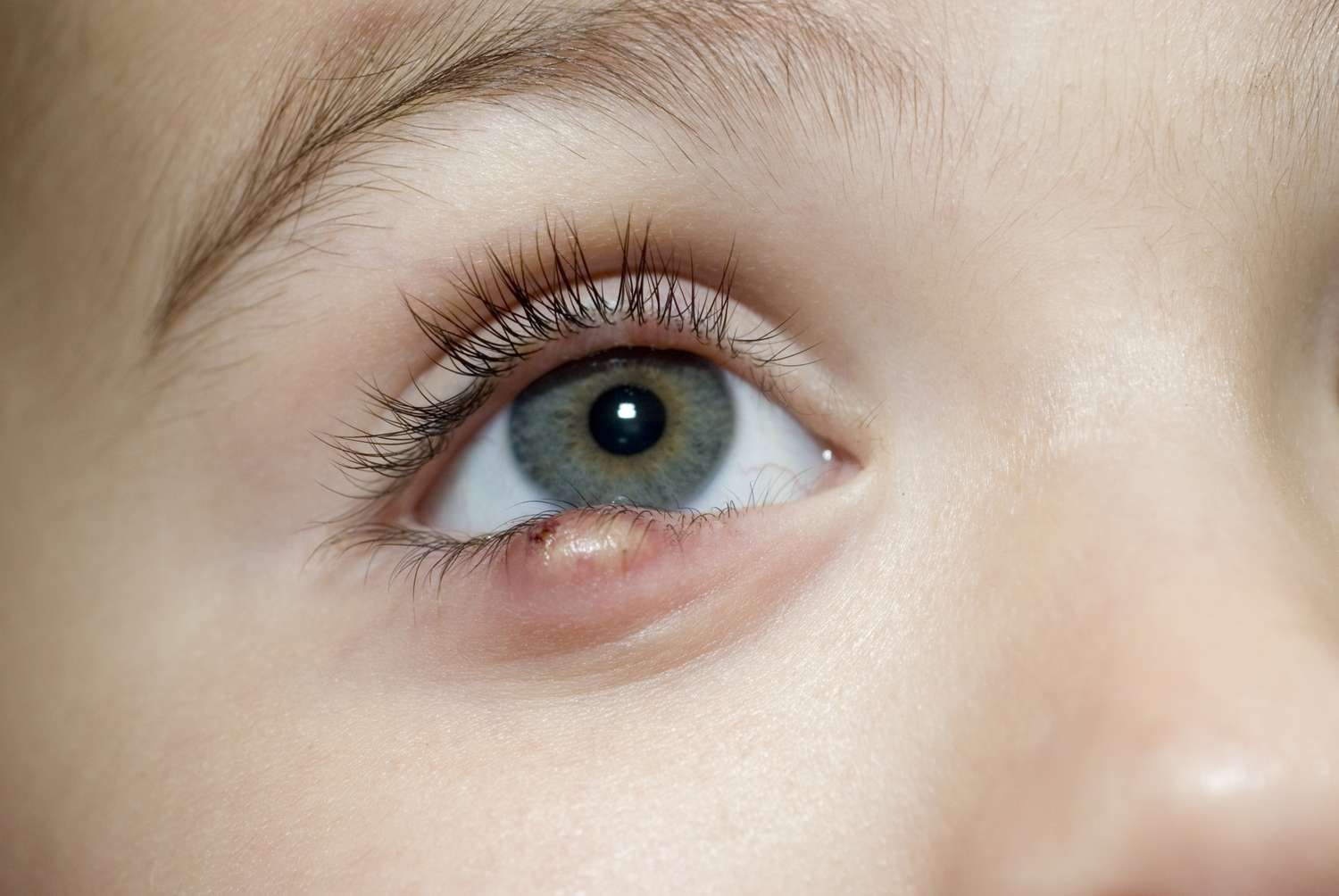
A stye (medical name: hordeolum) is a small, painful bump on the eyelid caused by an infected oil gland or hair follicle. It often looks like a pimple right along the eyelid margin (near the lashes), or a tender swollen area slightly farther up on the lid.
Styes are most often caused by Staphylococcus bacteria, which commonly live on the skin. That sounds alarming, but it is normal. A stye happens when bacteria and oil get trapped and an eyelid gland gets inflamed or infected.
External vs internal stye
- External stye: Usually near the lash line (often a lash follicle gland).
- Internal stye: Usually deeper in the lid (often a meibomian oil gland) and can look like more general lid swelling at first.
Home care is similar for both, but deeper (internal) styes can take longer to calm down.
Why do kids get styes?
Kids are basically professional face-touchers. Add in runny noses, sticky hands, and the occasional “I rubbed my eye with the sleeve I used to wipe the dog,” and you have the perfect setup.
Common causes
- Rubbing the eyes (especially with unwashed hands)
- Blepharitis (chronic eyelid inflammation with crusting at the lash line)
- Clogged oil glands in the eyelid
- Recent cold or allergies that lead to more eye-rubbing
- Skin conditions like eczema or seborrheic dermatitis
- Contact lenses (more common in older kids and teens), especially with poor lens hygiene
- Sharing towels or washcloths
Stye symptoms in kids
Most styes are easy to spot and come with a few classic symptoms.
- A red, tender bump on the eyelid
- Swelling of part of the lid
- Soreness, especially when blinking
- Watery eye or mild irritation
- A tiny white or yellow “head” may appear as it comes to the surface
Some kids also develop mild crusting along the lashes, especially in the morning.
If your child has diffuse redness of the white of the eye, lots of discharge, or both eyes are involved, that may be conjunctivitis instead of (or in addition to) a stye. When in doubt, check in with your clinician.
How long does a stye last?
With consistent warm compresses, many styes start to feel better within a few days. Most resolve in about 1 to 2 weeks, although some linger longer, especially if they are deeper in the lid or your child will not let you near their eye (solidarity).
If the bump is getting bigger after several days, not improving after about a week, or keeps coming back, it is time to check in with your child’s clinician.
Home treatment that helps
The most effective and safest home treatment is also the least glamorous: warm compresses. Warmth helps soften and open the clogged gland, encouraging it to drain naturally.
Warm compress steps
- Wash your hands.
- Wet a clean washcloth with warm (not hot) water.
- Wring it out and place it gently over the closed eyelid.
- Hold for 10 to 15 minutes.
- Re-warm as needed so it stays comfortably warm.
- Aim for 3 to 4 times per day. If you can do more, great. If you can only manage a couple minutes here and there, that still helps.
Gentle lid hygiene (if crusty)
If there is crusting on the lashes, you can gently clean the lid margin once or twice daily:
- Use a clean, warm washcloth and a tiny bit of baby shampoo diluted in water, or use a clinician-approved eyelid wipe (many families find wipes less irritating).
- Wipe gently along the lash line with the eye closed.
- Avoid getting soap in the eye, and stop if it seems to sting or irritate.
Pain relief
If your child is uncomfortable, age-appropriate acetaminophen or ibuprofen can be used as directed on the label (or as your clinician recommends). Warm compresses often help with pain too.
What not to do
- Do not squeeze or pop a stye. This can push infection deeper and worsen swelling.
- Do not use leftover antibiotic drops from an old eye infection unless your child’s clinician told you to.
- Avoid eye makeup (teens) until healed.
- Avoid contact lenses until the eye is comfortable and the stye is resolving.

Stye vs chalazion
These two get mixed up constantly, and they can look similar at first.
Stye (hordeolum)
- Usually painful and tender
- Often red and near the lash line
- Caused by an infection
- May develop a pimple-like head
Chalazion
- Usually not very painful (more of a firm lump)
- Often sits farther from the lash line, within the lid
- Caused by a blocked oil gland and inflammation, not an active infection
- Can last weeks to months
Warm compresses help both. A chalazion is more likely to need a clinician visit if it is large, persistent, affecting vision, or keeps returning.
When to call the doctor
Most styes can be managed at home, but there are times we want a clinician to take a look.
Call within 24 hours if:
- The swelling and redness are spreading beyond the eyelid, especially into the cheek or brow area
- Your child has fever or seems unusually ill
- The eyelid is very swollen or the eye is swollen shut
- There is significant eye pain, not just tenderness of the lid
- Your child has vision changes (blurry vision, double vision, trouble seeing)
- The eyeball itself looks very red, especially with light sensitivity
- Your child is a newborn or young infant
- Your child is immunocompromised (for example: on chemotherapy, post-transplant meds, high-dose steroids, or has a condition affecting immune function)
- The stye is not improving after 5 to 7 days of warm compresses
- Styes are recurrent or your child has frequent eyelid irritation
Go to urgent or emergency care now if:
- There is severe swelling with painful eye movement
- Your child cannot move the eye normally, or the eye looks like it is bulging (proptosis)
- There are new neurologic symptoms (severe headache, confusion) along with eye swelling
Those last symptoms can suggest a deeper infection around the eye, which needs prompt medical treatment.
What a clinician may recommend
Depending on what they see, your child’s clinician may recommend:
- Continue warm compresses (still the mainstay)
- Topical antibiotic ointment if there is drainage, significant crusting, or concern for bacterial involvement at the lid margin
- Oral antibiotics if there are signs of a spreading skin infection around the eye
- Referral to an eye specialist if the bump is persistent, recurrent, or suspicious for a chalazion that may need additional care
Rarely, a persistent or very large lesion may be drained in a controlled medical setting. Please do not attempt this at home.
If a bump keeps coming back in the same spot or does not resolve over time, your clinician may also consider other eyelid conditions. That is uncommon, but it is a good reason not to ignore persistent lumps.
Is a stye contagious?
The stye itself is not like viral pink eye, where watery discharge spreads easily. But the bacteria that contribute to styes can spread through shared towels, washcloths, pillowcases, and dirty hands.
If there is drainage, treat it as potentially contagious: be extra strict about handwashing and do not share anything that touches the face.
Simple precautions
- Teach and remind: hands off the eyes (I know, easier said than done).
- Use a fresh washcloth for compresses each time if possible, or wash it in hot water.
- Do not share towels, washcloths, eye makeup, or pillowcases.
- Change pillowcases every few days while it is healing.
Preventing repeat styes
If your child gets one stye and never sees another, wonderful. If they are a repeat offender, focus on the basics and a little eyelid hygiene.
- Handwashing before meals, after school, and after blowing the nose
- Address allergies so your child rubs less (talk with your clinician about options)
- Daily face washing, especially around the eyes
- If your child has frequent crusting: gentle lid cleaning a few times per week
- For contact lens wearers: strict lens hygiene and replacing cases regularly
- For teens: replace old eye makeup and avoid sharing it
One triage-nurse tip I wish I could put on a billboard: if your kiddo is rubbing their eyes a lot, that is your early warning sign. Treat the itch (allergies, dryness, irritation) and you often prevent the stye that follows.
Quick FAQ
Can I send my child to school with a stye?
Usually yes, if they feel well. Encourage handwashing and remind them not to rub their eye. If there is a lot of drainage, consider keeping them home until it is better controlled, and check your school’s policy.
Should I use an eye patch?
No. Patching can trap moisture and bacteria and may make things worse.
Can a stye cause blurry vision?
A large swollen lid can make vision seem blurry simply because it is in the way. True vision changes are a reason to call your clinician.
What if the bump “pops” on its own?
That can happen. Gently clean any drainage, keep doing warm compresses, and wash hands well. Call your clinician if redness is spreading or your child seems worse.
Bottom line
Styes are common in kids, usually mild, and typically improve with warm compresses and a little patience. If your child has spreading redness, fever, significant pain, vision changes, or the stye is not improving after about a week, get medical guidance so you are not guessing.
You are not doing anything wrong if your child gets a stye. You are parenting a tiny human with hands that are always mysteriously sticky. We work with what we have.