Tinea Versicolor in Kids
Sarah Mitchell
Sarah Mitchell is a Registered Pediatric Nurse and a mother of three who has spent over a decade helping families navigate the beautiful, chaotic early years of childhood. She combines evidence-based medical knowledge with real-world parenting experience to offer practical, compassionate advice. At Awesome Parent, Sarah's mission is to help exhausted parents find solutions, trust their instincts, and finally get some sleep.
If you have ever put sunscreen on your child and suddenly noticed faint patches you swear were not there yesterday, you are not alone.
This is one of those very common, very fixable skin things that tends to show up at the worst time, like right before swim lessons or family photos.
One likely culprit is tinea versicolor (also called pityriasis versicolor). Despite the word “tinea,” it is not the same as ringworm. It is a yeast that normally lives on skin but can overgrow and cause patchy color changes. It is usually harmless, but it can definitely be annoying and confidence-shaking.

What it is (and why it shows up)
Tinea versicolor is caused by an overgrowth of a yeast (Malassezia) that naturally lives on most people’s skin. When it grows a little too enthusiastically, it can interfere with normal pigment and create patches that look lighter, darker, or slightly pink compared with the surrounding skin.
Common triggers in kids
- Heat and humidity (summer, sweaty sports, tropical vacations)
- Sweating and not changing out of damp clothes quickly
- Oily skin
- Heavy, occlusive lotions that may trap heat and moisture (not always a trigger, but it can contribute for some kids)
- Hormonal changes (more common in tweens and teens, but younger kids can get it too)
- Weakened immune system or certain medicines (less common, but worth mentioning to your clinician)
It is not a sign of poor hygiene, and it is not something you “caused.” It is one of those “skin microbiome got out of balance” situations.
What the spots look like
This is the classic story: your child tans a bit, and suddenly you notice lighter patches that did not tan. That happens because the affected areas do not pigment the same way as the surrounding skin.
Typical appearance
- Flat patches (not raised like welts)
- Color change: lighter, darker, pink, or coppery
- Fine, dry scale that can look like “dusty” skin, especially if you gently scratch or rub it
- Most common locations: chest, back, shoulders, upper arms, sometimes neck
- Usually mild itch or none at all
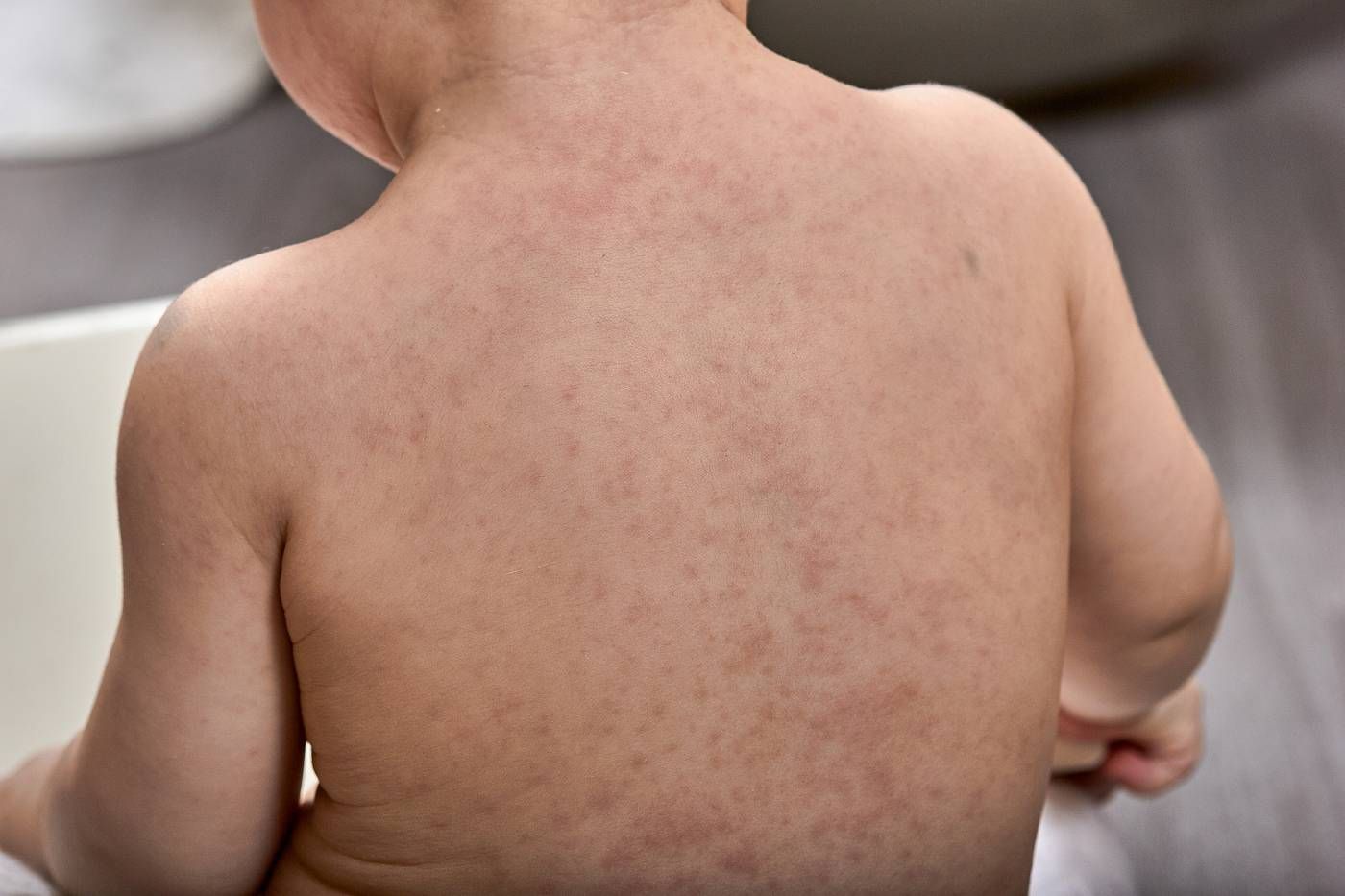
How it looks on different skin tones
This is where a lot of families get understandably confused. The yeast does not choose one “look.” It creates contrast.
- On lighter skin tones, patches may look slightly darker, pinkish, or tan.
- On medium to deeper skin tones, patches often look lighter (hypopigmented) and can be more noticeable after sun exposure.
- On very deep skin tones, patches may appear ashier or “washed out,” sometimes with a soft border rather than a sharp ring.
Important reassurance: even after the yeast is treated, the color can take weeks to months to fully blend back in. That pigment recovery is slow and it does not mean treatment failed.
One practical tip while you wait: sun protection can reduce contrast. It will not cure the rash, but it can make the patches less obvious while skin tone evens out.
Why it comes and goes
Tinea versicolor loves warm, humid conditions, so it often flares in late spring and summer and calms down in cooler months. Some kids get a “repeat performance” every year, especially if they sweat a lot or live in humid climates.
If your child tends to get it repeatedly, your pediatrician or dermatologist may recommend a simple prevention routine during warm months.
OTC treatment options
For most otherwise healthy kids with a typical rash, you can start with over-the-counter antifungal options. The goal is to reduce the yeast on the skin.
Quick safety callout: Avoid using steroid creams (like hydrocortisone) on a rash you suspect is fungal unless your child’s clinician tells you to. Steroids can sometimes make fungal rashes harder to clear.
Good OTC choices
- Selenium sulfide shampoo (often marketed for dandruff)
- Ketoconazole shampoo (availability varies by country and store)
- Zinc pyrithione shampoo
- Topical antifungal creams like clotrimazole or miconazole for smaller areas
Using shampoo as a body wash
This is a common, clinician-recommended approach for larger areas on the chest or back:
- Apply a small amount to the affected skin in the shower.
- Leave it on for about 5 to 10 minutes (long enough to work without turning bath time into a detangling drama, short enough to keep everyone sane).
- Rinse well.
- Repeat for 1 to 2 weeks, or exactly as the label and your clinician recommend. Some regimens use it daily, others a few times per week.
Safety note: Avoid getting these products into eyes, and do not use on broken or very irritated skin unless your child’s clinician says it is okay. Also, follow pediatric labeling closely, especially for younger children. If your child has very sensitive skin or eczema, creams may be gentler than medicated shampoos.
When you should see improvement
The fine scale often improves within a week or two. The color change can lag behind for quite a while, especially after sun exposure. If the patches are no longer spreading and the scale is gone, that is often a good sign you are on the right track.
Prescription options
If OTC treatment is not helping, the rash is widespread, or you are not sure of the diagnosis, it is time to check in with your child’s clinician. They may prescribe:
- Stronger topical antifungals (creams, foams, or washes)
- Prescription-strength ketoconazole wash or shampoo
- Oral antifungals for severe or stubborn cases (used selectively in kids and guided by a clinician)
If an oral medicine is considered, clinicians typically choose options with safer pediatric track records. Oral ketoconazole is generally avoided in many guidelines because of the risk of serious liver injury.
How clinicians confirm it
In clinic, a clinician can often identify tinea versicolor by the look and feel (including that fine scale). If the diagnosis is unclear, they may do a quick, painless skin scraping and look at it under a microscope (a KOH test). Sometimes a Wood’s lamp (special light) is used and may show a subtle yellow-green or coppery glow.
Look-alikes to know
This is the part I used to walk families through at triage, because the treatments are not identical. If you are not sure, it is always reasonable to check in before you treat.
Tinea versicolor vs ringworm
- Tinea versicolor: usually many small or medium patches, often on chest and back, with fine scale and soft borders.
- Ringworm (tinea corporis): tends to be one or a few round or oval rings with a more defined border and clearing in the center. Can be itchier. Often on arms, legs, or face. Can spread from pets, wrestling mats, or close contact.
Ringworm is also a fungus, but it is a different one. It usually needs a true antifungal cream applied consistently, and scalp involvement needs prescription treatment.
Tinea versicolor vs eczema
- Tinea versicolor: pigment change with fine scale, often minimal itch, more common on trunk.
- Eczema: typically very itchy, red and inflamed during flares, may ooze or crust, and often shows up in skin folds (behind knees, inside elbows) depending on age.
Eczema is not caused by yeast overgrowth on the skin surface. Using steroid cream on what is actually a fungal rash can sometimes make the fungal rash worse, so it is worth getting clarity if you are unsure.
Two other common possibilities
- Pityriasis alba: lighter, slightly scaly patches, often on the face in children. It is often linked with dry skin or eczema.
- Vitiligo: well-demarcated patches of pigment loss that look brighter white and do not have scale.
Can it spread?
Tinea versicolor is generally considered not very contagious. The yeast is commonly present on many people’s skin already. The issue is overgrowth, not catching it from someone else. Siblings do not usually need treatment unless they have their own rash.
When to call the pediatrician
Please get your child checked if:
- The spots are on the face and spreading quickly
- There is pain, swelling, pus, warmth, or honey-colored crusting
- Your child has a fever or seems unwell
- The rash is very itchy or disrupting sleep
- OTC treatment has not helped after 2 to 3 weeks
- Your child is immunocompromised or has a complex medical history
No scary procedures required. Most of the time, it is a quick exam, and sometimes a simple scraping or special light to confirm.
Keeping it from coming back
Some kids get one episode and never see it again. Others get it every summer. If your child is in the repeat club, these steps can help:
- Change out of sweaty clothes soon after sports or camp.
- Use lightweight, breathable fabrics in hot weather.
- Skip heavy, oily lotions on the chest and back during humid months.
- Ask your clinician if a once-weekly medicated wash during summer makes sense for your child.
And the most important reminder: even when the yeast is gone, the “tan lines” can linger. That is normal. Your child’s skin is not permanently damaged, it just needs time to even out.
Quick recap
- Tinea versicolor is a common yeast overgrowth that causes light, dark, or pink patches, often on the trunk.
- It frequently becomes noticeable after sun exposure because affected areas tan differently.
- OTC antifungal shampoos used as body wash and antifungal creams often help. Follow the label and age guidance.
- Color can take weeks to months to normalize after treatment.
- See your pediatrician if it is spreading fast, looks infected, is very itchy, or is not improving.
If you are staring at your kid’s shoulders under the bathroom light wondering if you missed some new and exotic disease, take a breath. Most of the time, this is straightforward, treatable, and more annoying than dangerous.