UTI in Toddlers: Signs, Causes, and When to See a Doctor
Sarah Mitchell
Sarah Mitchell is a Registered Pediatric Nurse and a mother of three who has spent over a decade helping families navigate the beautiful, chaotic early years of childhood. She combines evidence-based medical knowledge with real-world parenting experience to offer practical, compassionate advice. At Awesome Parent, Sarah's mission is to help exhausted parents find solutions, trust their instincts, and finally get some sleep.
If your toddler has a fever and you cannot find a runny nose, cough, or other obvious source to explain it, a urinary tract infection (UTI) is one of the big things we want on the checklist. UTIs are common in little kids, and they can be sneaky, especially when your child cannot tell you, “It burns when I pee.”
As a pediatric nurse and a mom of three, I will tell you this upfront: you are not overreacting by asking about a UTI. Catching and treating one early matters, because untreated UTIs can sometimes spread upward to the kidneys and make kids very sick.

What is a UTI?
A UTI is an infection anywhere in the urinary system:
- Bladder infection (cystitis): More common. Often causes urinary symptoms like pain, urgency, and accidents.
- Kidney infection (pyelonephritis): More serious. Often causes higher fever and more “whole body” illness.
Most UTIs in children are caused by bacteria (often E. coli) that get into the urethra and travel up into the bladder.
UTI signs in toddlers
Toddlers are famous for giving us vibes instead of details. Here are the most common clues parents notice.
Signs that can look random
- Fever with no clear source (no obvious cold symptoms, no clear stomach bug signs, no known reason).
- New crankiness or low energy, clinginess, or “off” behavior.
- Eating less or drinking less.
- Vomiting or belly pain, sometimes with fever.
More specific pee clues
- Crying, wincing, or trying to hold it during urination.
- Urgency or frequency (needing to go right now, or going over and over).
- Foul-smelling urine that is noticeably different than usual.
- Cloudy urine or blood-tinged urine (pink-tinged). If urine looks very dark (cola or tea-colored), call your clinician promptly because other issues can cause that too.
- Potty training regression, new daytime accidents, or bedwetting after doing well.
- New genital grabbing or saying “owie” in the diaper area.
Signs that suggest a kidney infection
- Higher fever (often 101 to 102°F or higher, but not always).
- Back or side pain (your toddler may point to their side/back or refuse to be touched there).
- Looks more ill: very low energy, pale, or hard to comfort.
Nurse triage note: “Fever with no source” in a toddler is one of the most common ways UTIs show up. If your gut is telling you something is off, trust it and call.
What causes UTIs in toddlers?
UTIs are not caused by being “dirty” or by parents doing something wrong. They are usually a perfect storm of toddler anatomy, bathroom habits, and bacteria that live around the bottom.
Common risk factors
- Wiping issues: For kids with vulvas, wiping back-to-front can move bacteria toward the urethra. This is very common during the learning phase.
- Constipation: A big one. Stool in the rectum can press on the bladder, lead to incomplete emptying, and increase bacteria around the area.
- Holding pee: Toddlers get busy and ignore the urge to go, especially during play or early potty training.
- Not fully emptying the bladder: Quick “tinkle and run” potty visits can leave urine behind where bacteria can grow.
- Diapers and moisture: Wetness and irritation can make the area more vulnerable for some kids. Diapers do not “cause” UTIs, but diaper life can add to the perfect storm.
- Bubble baths and irritants: These can irritate the urethra for some kids and make symptoms more noticeable.
- Being uncircumcised: Uncircumcised boys have a slightly higher UTI risk in infancy; after infancy, the difference is smaller.
- Urinary tract differences (anatomy): Some kids have reflux of urine toward the kidneys (vesicoureteral reflux) or other structural issues that raise risk.

When to call the doctor
Call within 24 hours if your toddler has:
- Fever without a clear source, especially if it lasts more than a day.
- Painful urination, urgency/frequency, or new accidents.
- Foul-smelling urine plus any other symptoms (fever, fussiness, belly pain).
- A history of UTIs and similar symptoms returning.
Seek urgent or emergency care now if:
- Your child is under 3 months with any fever (this is always urgent).
- Your toddler looks very ill, very sleepy, hard to wake, or is struggling to breathe.
- They cannot keep fluids down, have repeated vomiting, or show signs of dehydration (dry mouth, no tears, very little urine).
- They have severe belly or back pain with fever.
- You suspect a kidney infection and your child is worsening quickly.
If you are on the fence, it is absolutely appropriate to call your pediatrician’s nurse line. This is exactly what it is for.
How a UTI is diagnosed
To truly confirm a UTI, clinicians rely on a urine test from an appropriately collected sample, usually a urinalysis (UA) plus a urine culture. Symptoms alone are not enough, because other things can mimic a UTI.
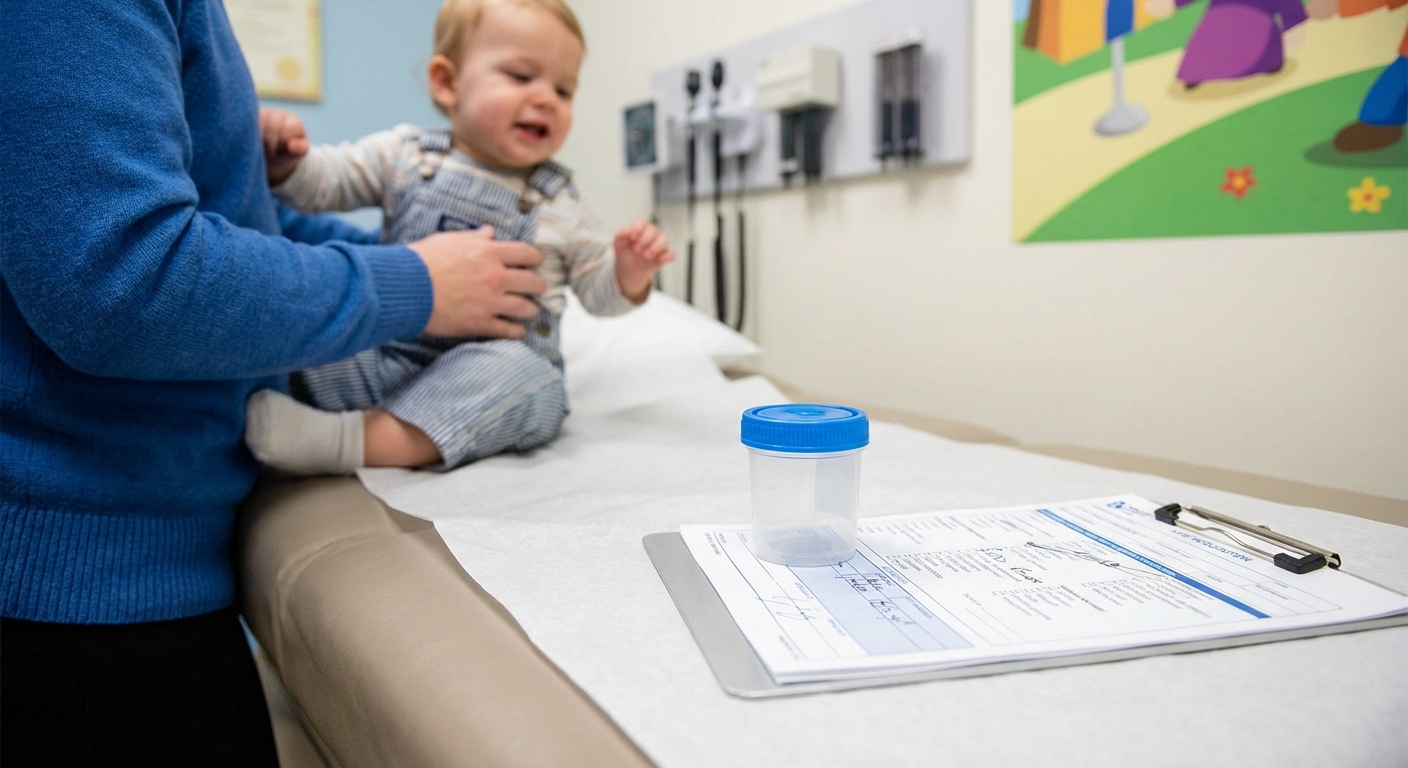
Step 1: Getting a urine sample
How the urine is collected matters a lot, because contamination can make results confusing.
- Clean-catch urine (toilet-trained toddlers): The genital area is cleaned, then urine is collected midstream in a sterile cup. This is often the first choice if your child can cooperate.
- Catheterized sample (common for non-toilet-trained kids): A tiny catheter is used to collect urine directly from the bladder. It is quick and gives a clean sample, which helps avoid false positives.
- Urine bag (screening only): A sticky bag catches urine in diapers. Because it touches skin, it is more likely to be contaminated. A negative result can be helpful to rule out UTI, but a positive bag test is not diagnostic and is usually confirmed with a catheter sample (or, in young infants, sometimes a suprapubic aspiration).
Parent tips for sample day
- Hydrate early: Offer water on the way in so they are more likely to pee.
- Bring comfort: A familiar stuffed animal or a quick video can help during a cath.
- Ask your team to talk you through it: A calm, quick plan helps toddlers cooperate.
- If clean-catch is the plan: Ask if they want you to start collecting midstream. Little details matter for accuracy.
Step 2: UA and culture
- Urinalysis (UA): A quick test that looks for signs of infection like white blood cells, nitrites, and leukocyte esterase. UA can be strongly suggestive, but it is not the final word by itself.
- Urine culture: Grows bacteria to confirm infection and show which antibiotic works best. Results often start coming back in 1 to 3 days, with final susceptibilities sometimes taking a bit longer depending on the lab.
Sometimes your child will start antibiotics before the culture is final, especially if they have fever or look unwell. The medication may be adjusted once culture results are back.
Important safety note: When possible, clinicians prefer to collect urine before starting antibiotics, because antibiotics can affect results. Also, do not use leftover antibiotics from a previous illness.
What else can mimic a UTI?
This is why we test. A few common look-alikes in toddlers include:
- Viral illness causing fever without urinary symptoms.
- Vulvovaginitis or irritant rash (soap, bubble baths, tight clothing, wiping irritation) that causes burning or grabbing.
- Constipation causing belly pain, accidents, and frequent small pees.
- Dehydration causing strong-smelling, darker urine and crankiness.
- Pinworms causing nighttime itching and irritation near the bottom.
Treatment: What to expect
Most toddler UTIs are treated with an oral antibiotic at home.
Typical treatment plan
- Antibiotics: The exact choice depends on local resistance patterns and your child’s urine culture. Bladder infections and kidney infections may need different durations, and febrile UTIs in younger children sometimes come with closer follow-up.
- Fever and pain support: Your pediatrician may recommend acetaminophen or ibuprofen (if age-appropriate) for comfort and fever.
- Hydration: Encourage fluids. More urine flow helps flush bacteria.
At-home tips that help
- Give the antibiotic exactly as prescribed and finish the course, even if your child seems better quickly.
- Expect improvement within 24 to 48 hours after starting antibiotics. If fever or pain is not improving, call back.
- Do not rely on cranberry products as treatment. They are not a substitute for antibiotics when there is a bacterial infection.
Real-life parenting note: If your toddler suddenly refuses to pee because it hurt once, that is common. Warm baths (no bubbles) can relax them, and pain control per your clinician’s guidance can make the next bathroom trip less scary.
Repeat UTIs
Some toddlers get more than one UTI. If your child has recurrent infections, your pediatrician may look for contributing factors and, in some cases, recommend imaging.
Why UTIs come back
- Constipation that is not fully addressed.
- Bladder habits like holding urine or not fully emptying.
- Wiping skills (developmentally normal, just needs support).
- Anatomic differences such as vesicoureteral reflux.
Possible next steps
- Kidney and bladder ultrasound: A painless scan to look at anatomy and check for blockage or other concerns. Often considered after febrile UTIs in young children or recurrent UTIs, depending on age and history.
- Additional tests: In selected situations, your clinician may consider studies to evaluate reflux or bladder function.
If your toddler has repeat infections, ask your pediatrician, “What is our plan to prevent the next one?” That question opens the door to the most helpful stuff: constipation management, pee schedules, and targeted follow-up.
Prevention tips
You do not need a complicated routine. Small habit changes make a big difference, especially if your child is prone to UTIs.
Bathroom habits
- Regular potty breaks: Aim for every 2 to 3 hours while awake. Toddlers rarely self-schedule well.
- Take time to fully empty: Encourage a pause and try again at the end. Some families call it “double pee.”
- Relaxed posture on the toilet: Feet supported on a stool helps pelvic muscles relax.
Wiping and hygiene
- Front to back wiping for kids with vulvas. In the early days, you may need to help or do a final parent wipe.
- Skip bubble baths if your child is sensitive or has had UTIs.
- Choose gentle soap and avoid scrubbing the genital area. Warm water is often enough.
- Change wet or soiled underwear promptly.
Constipation prevention
- Watch stool patterns: Hard stools, painful poops, skipping days, or poop smears in underwear can all signal constipation.
- Fiber and fluids: Fruits, veggies, whole grains, and water help.
- Talk with your pediatrician if constipation is ongoing. Improving constipation can meaningfully lower the risk of repeat UTIs for many kids.
Hydration
- Offer water throughout the day.
- For some kids, a fun cup or a straw helps.

Common 3 AM questions
Can a toddler have a UTI without pain?
Yes. Some toddlers mainly show fever, fussiness, belly pain, vomiting, or a sudden change in potty habits.
Does foul-smelling urine always mean a UTI?
No. Dehydration, certain foods, and vitamins can change urine odor. But if the smell is new and strong plus there are other symptoms (fever, accidents, pain), it is worth testing.
Is a UTI contagious?
No, UTIs are not spread like colds. They are typically caused by a child’s own bacteria getting into the urinary tract.
Can potty training cause UTIs?
Potty training does not directly cause UTIs, but the phase can increase risk because kids may hold urine, rush bathroom trips, or have more constipation. A gentle schedule and constipation prevention go a long way.
Bottom line
UTIs in toddlers are common and treatable, but they can be hard to spot. If your toddler has fever with no obvious source, cries with urination, has foul-smelling urine, or suddenly backslides in potty training, it is reasonable to ask for a urine test. You are not being “that parent.” You are being the parent who catches things early.
If you are heading to the doctor, it helps to bring these details: your child’s age, how long the fever has lasted, whether they are potty trained, how often they are peeing, any accidents, any belly or back pain, any constipation, and whether they have had a UTI before.